An 11-year-old boy from Dubai presented to the outpatient department with a history of penoscrotal hypospadias which was repaired at the age of 3 years. The patient had no urinary complaints, but parents had noted a thin urinary stream. The biggest concern for the parents was the appearance of the penis, they described it as buried and small. On physical examination, there was a buried penis with meatus located at the glans tip (suggesting previous urethral reconstruction). But the child had a significant penile curvature (chordee)- more than 90 degrees which meant that during previous surgery chordee correction was not performed. After detailed counselling and discussion with the family we went ahead with staged reconstructive surgery.
Stage 1 Surgery: Chordee Correction
A diagnostic cystoscopy was performed at the beginning of the procedure to evaluate the previously reconstructed urethra. The urethra was found to be narrow and strictured, confirming the need for revision. Surgery was initiated by marking the circumferential degloving incision. Local infiltration with xylocaine and adrenaline was administered at the marked site to aid hemostasis and analgesia. A deep degloving was then performed. Intraoperative assessment revealed severe chordee (>60° curvature). The corpus spongiosum was carefully mobilized on both sides, and the narrow, fibrotic urethra was divided in the distal penile region. The urethra was further mobilized proximally up to the penoscrotal junction. Following urethral division, chordee was reassessed and noted to have improved to <20°, indicating that the fibrotic urethra was a major contributing factor to the curvature. Thus, the initial severe chordee was effectively reduced to mild curvature after
urethral release. Subsequently all ventral fibrotic bands were completely excised This resulted in complete correction of chordee. Due to significant ventral fibrosis, we decided not to place a graft during this stage, to optimize tissue conditions for future reconstruction. The ventral penile skin was closed primarily. At the end of Stage 1, the meatus had receded to the perineal region.
Stage 2 Surgery: Oral Mucosa Graft (OMG) placement
The second stage of reconstruction was planned 6 months after Stage 1 to allow for complete healing, tissue maturation, and reorganization of the penile skin. At follow-up, the penis showed soft and supple skin on the ventral side with no residual chordee. This confirmed readiness for oral mucosa graft (OMG) placement. A midline incision was made along the ventral aspect of the penis, and the skin was carefully mobilized on both sides. A well-vascularized tunical bed was prepared to receive the graft. The urethral meatus was circumferentially mobilized to facilitate proper graft placement. Oral mucosa grafts were harvested from the right and left cheeks, measuring approximately 6 × 2 cm each. The graft
was placed over the prepared tunical bed. It was secured from the tip of the glans to the region surrounding the meatus. The graft edges were sutured to adjacent penile skin. Quilting sutures (5-0 vicryl) were used to fix the graft to the tunica, ensuring stability and optimal graft uptake. Three weeks after graft placement, topical steroid massage was initiated to improve graft pliability and prevent contraction. This was advised to continue for 5 months. However, due to irregular compliance, partial graft contraction occurred, particularly involving the midpenile and distal penile segment.
Revision of contracted graft
The contracted and unhealthy portion of the graft was surgically excised. A secondary oral mucosa graft was then harvested from the lower lip and placed in the affected region. This graft demonstrated good uptake and healing. Following successful graft revision, the surgical team waited one year to allow the graft to become soft, supple, and well- vascularized to achieve optimal graft condition for urethroplasty.
Stage 3: Urethroplasty
The final stage of reconstruction involved definitive urethroplasty, performed over a 12 Fr silicone catheter. An incision was made along the edges of the previously placed oral mucosa graft along with the overlying skin. The tissues were carefully deepened and mobilised to allow tension-free tubularization. The urethral reconstruction was performed in multiple layers. The first layer was closed in a continuous subcuticular fashion using 5-0 Vicryl. A second reinforcing layer was placed using interrupted sutures for added strength. To provide additional support and reduce the risk of fistula formation, a well-vascularized dartos flap was mobilized bilaterally and interposed over the neourethra. The glans wings were widely mobilized, and a glansplasty was performed to achieve a natural and conical glanular configuration. The penile skin was then closed in two layers with meticulous approximation. Given the complexity and length of reconstruction in a prepubertal child, a suprapubic catheter (SPC) was placed at the end of the procedure. The per urethral catheter was kept clamped. Urine drainage was maintained exclusively through the SPC to minimize pressure on the repair. In the postoperative period, the patient received 7 sessions of hyperbaric oxygen therapy (HBOT) to enhance wound healing and reduce complications. Dressing changes were performed every 4 days with thorough betadine cleansing. The per urethral catheter was removed on postoperative day 18 after confirming satisfactory healing. The suprapubic catheter was removed on postoperative day 21, once the child demonstrated good, unobstructed urinary flow per urethra.


Picture 1: Clinical picture showing completely buried penis with meatus at the tip
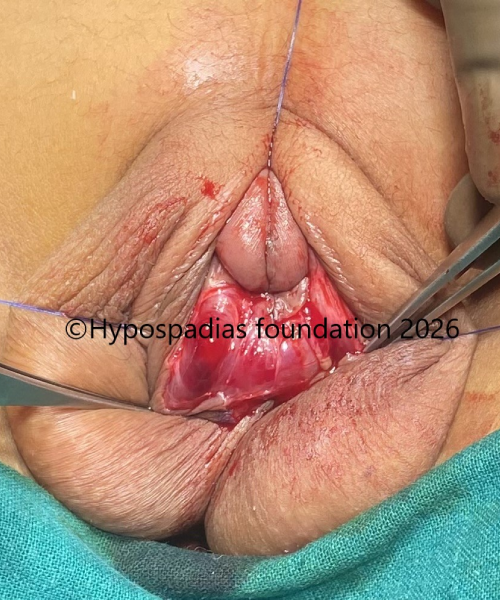
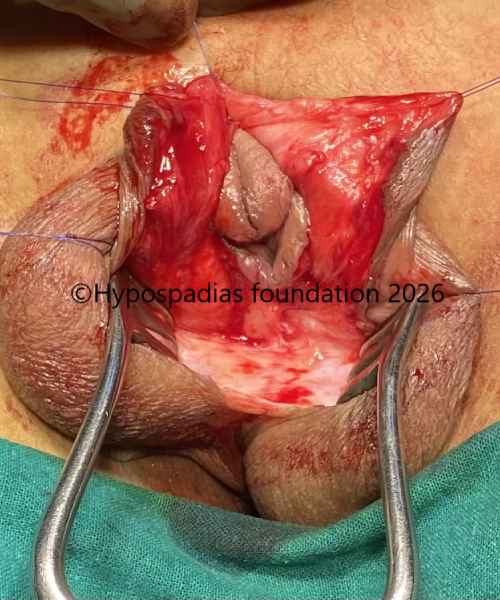
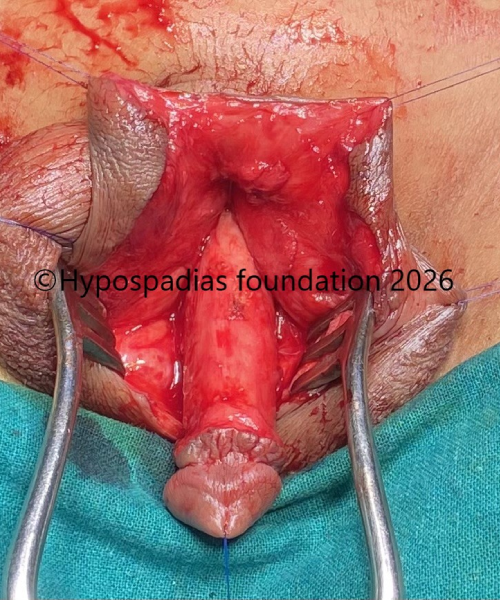
Fig 2: Complete degloving done and excessive fibrosis noted on the ventral side, causing the penis to get uried within
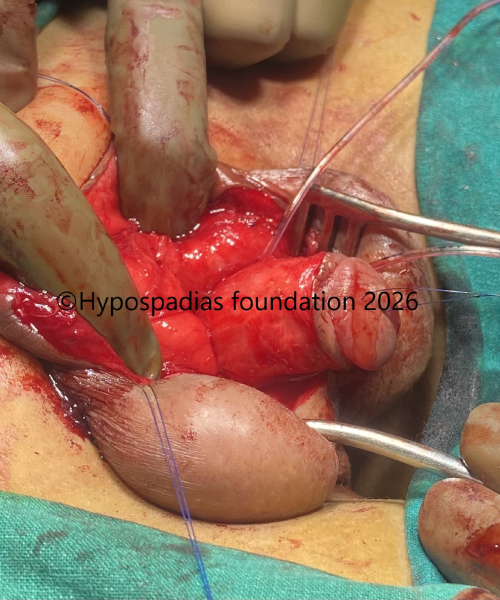
Fig 3: Chordee was assessed by artificial erection test and significant chordee of more than 60 degree was noted. Spongiosum was mobilized on either side, urethra was divided and proximal urethra was mobilized.
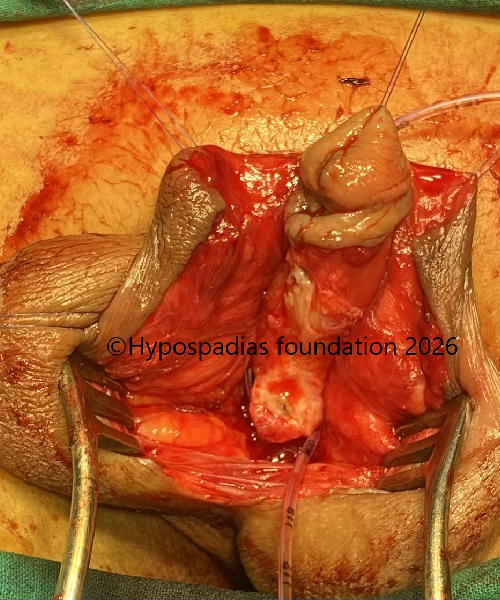
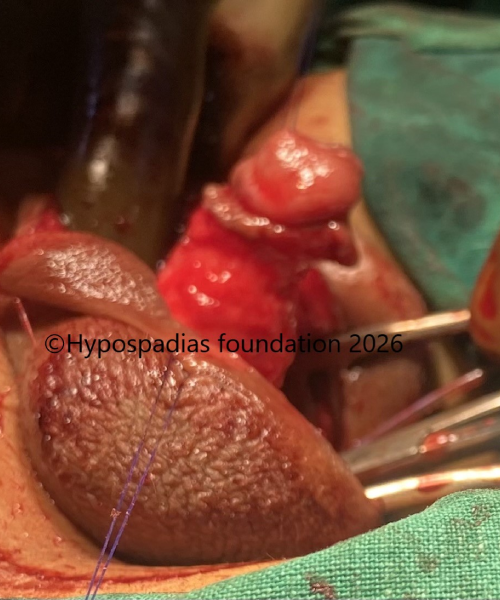
Fig 4: Chordee was completely corrected only by urethral plate division, and urethra receded to the perineal region.
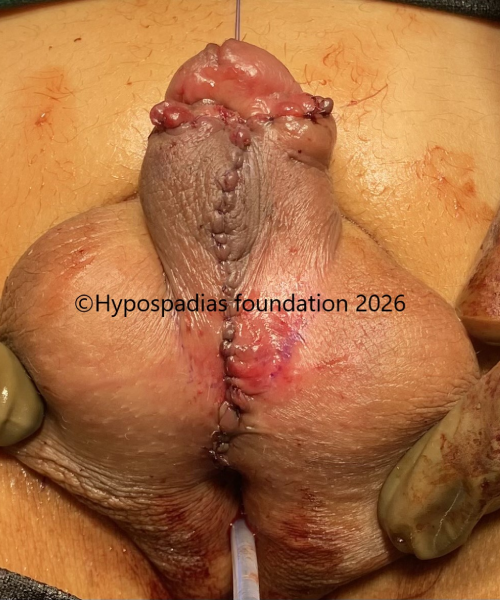
Fig 5: Since there was extensive fibrosis on the ventral side, we planned to only rearrange the skin in this stage and decided to place the oral mucosa graft in second stage. The above picture is appearance at the end of stage 1 chordee correction
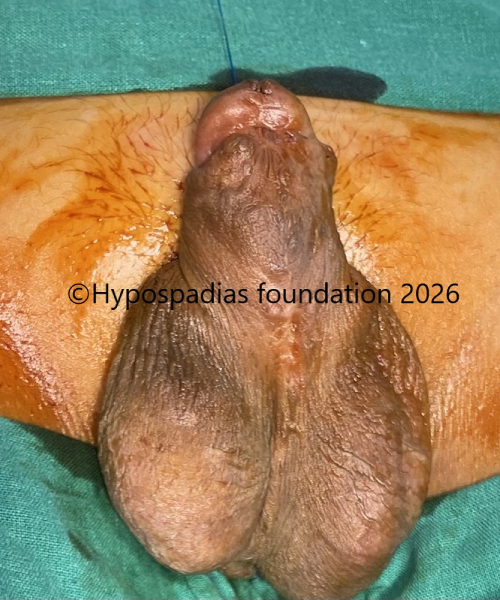
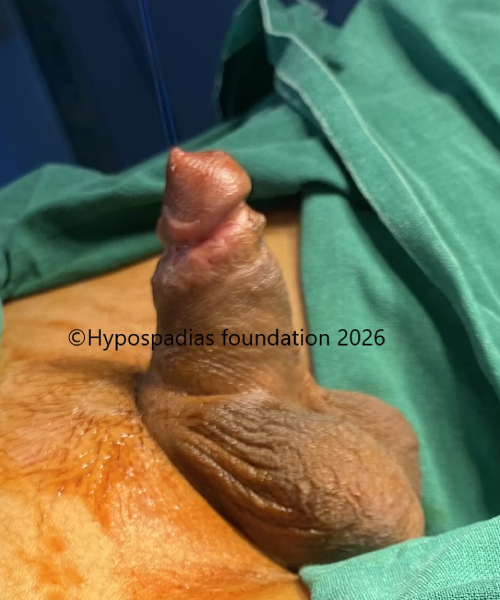
Fig 6: Intraoperative assessment before placing oral mucosa graft showed skin on the ventral side had healed well and there was no residual chordee
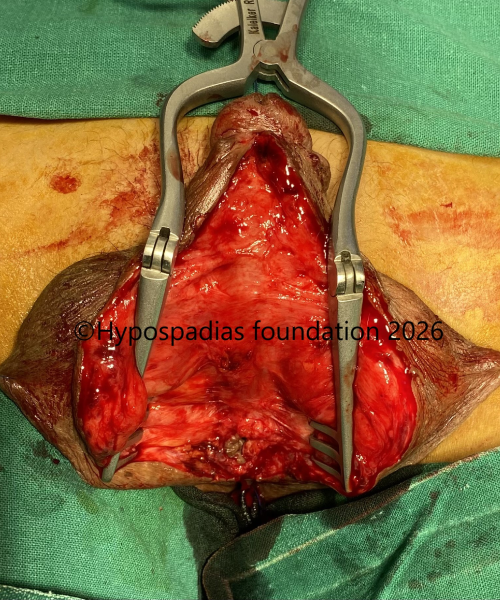
Fig 7: Midline incision was given and skin mobilized for placement of oral mucosa graft
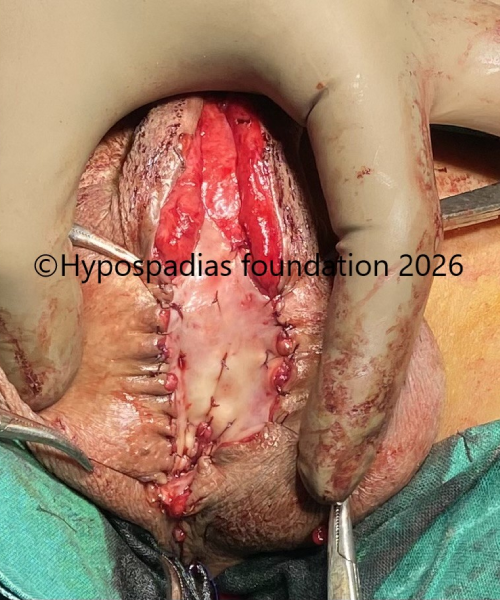
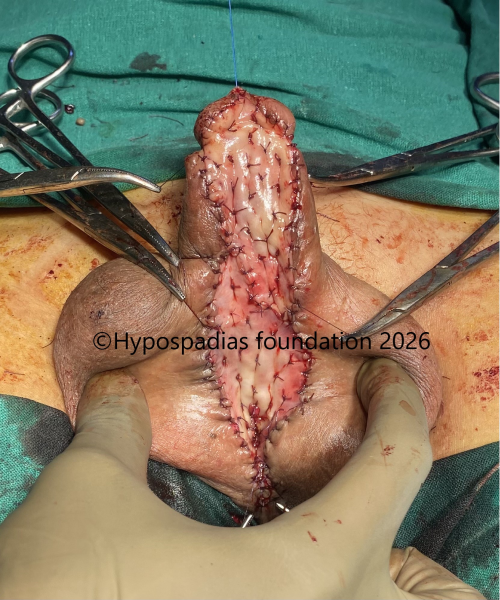
Fig 8: Oral mucosa graft was harvested from both cheeks and placed from the glans till all around the meatus. Post surgery, pressure dressing was done.
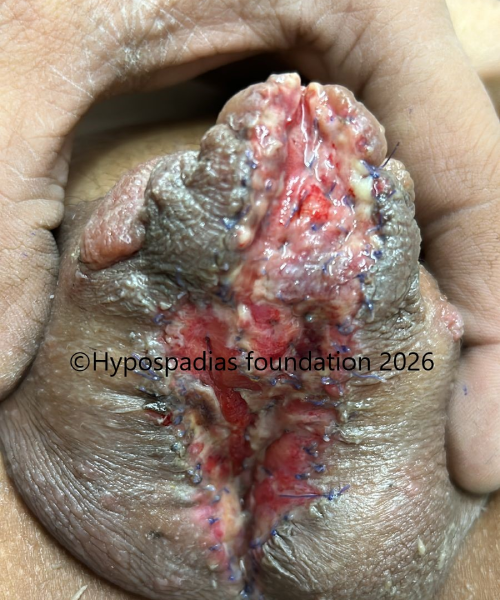
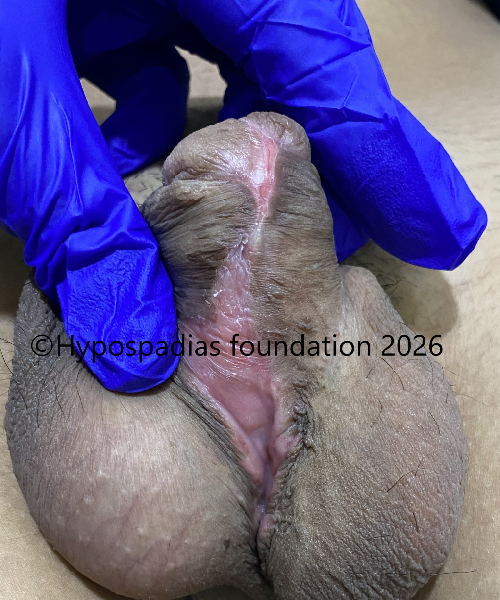
Fig 9: Dressing was removed on post operative day 7. Assessment done at 3 months after surgery showed that graft upto the proximal penile was good with 100% uptake but beyond this the graft had contracted. Hence was planned for distal oral mucosa graft augmentation
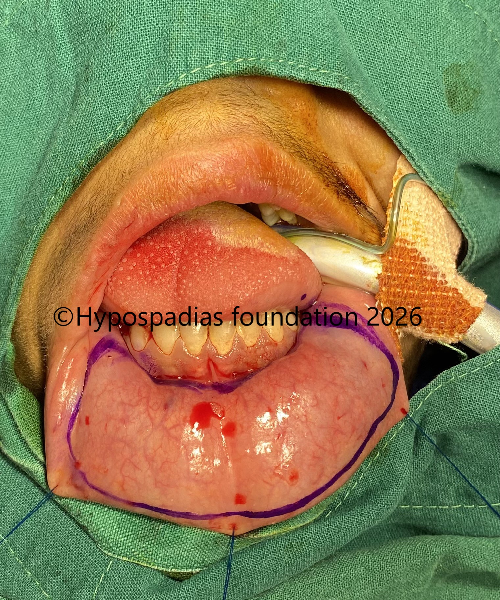
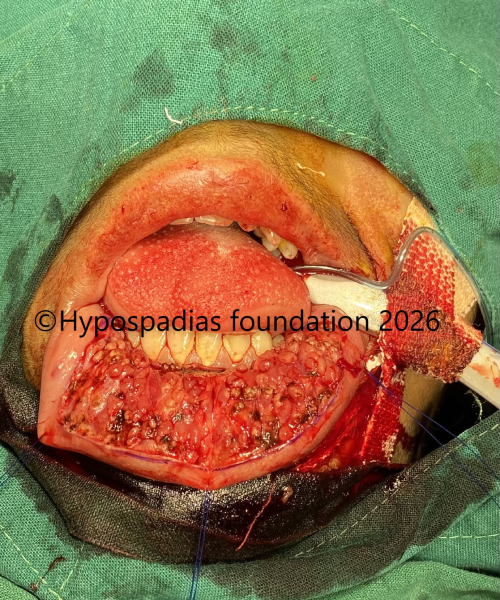
Fig 10: Oral mucosa graft harvested from lower lip
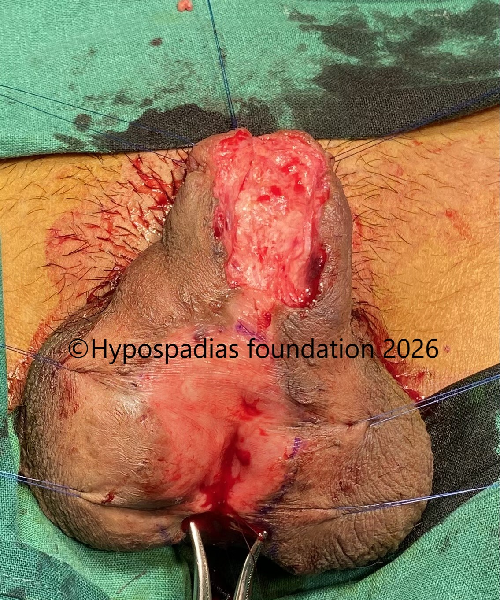
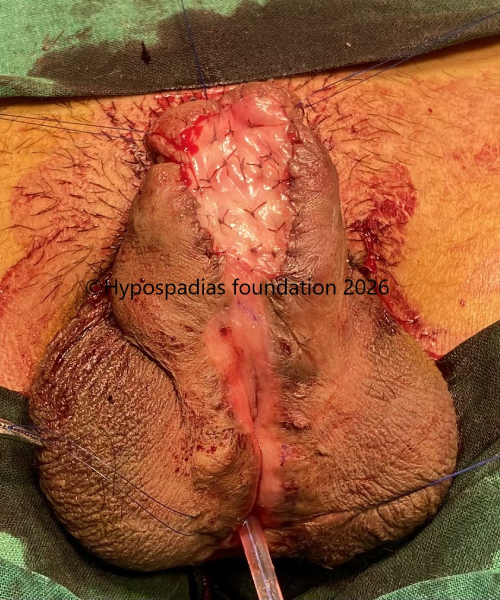
Fig 11: Distal contracted graft completely removed. Graft from lower lip sutured from the proximal penile to glans and quilted with 5-0 vicryl
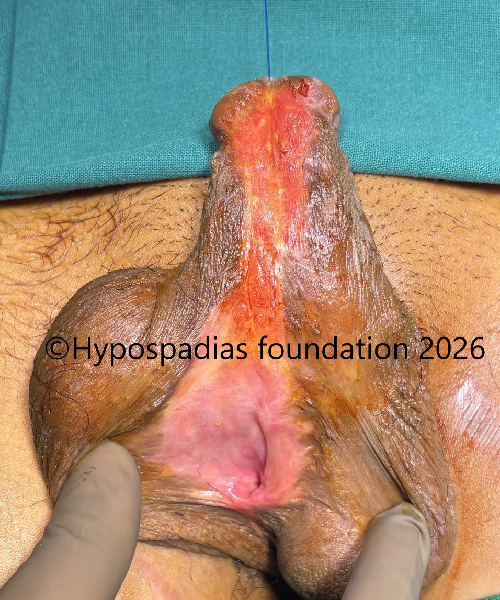
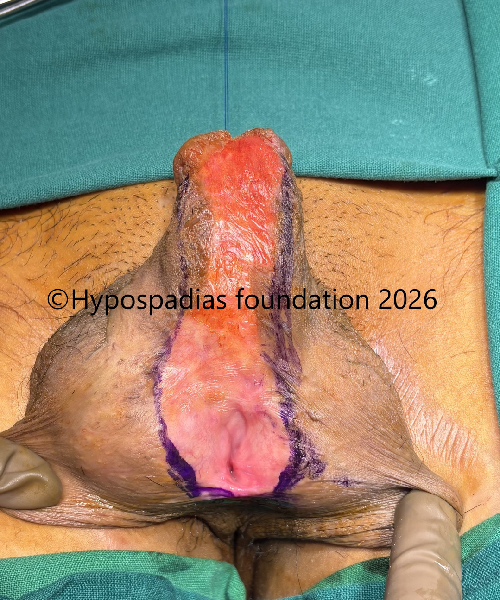
Fig 12: Redo graft uptake was good, and he was planned for stage 2 OMG urethroplasty. Marking done at the edges of the graft.
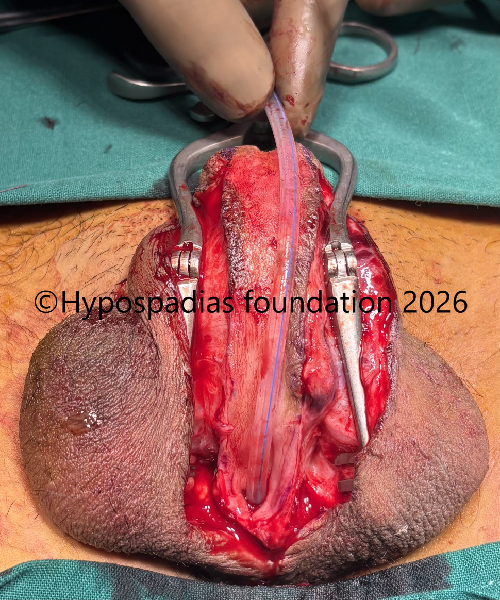
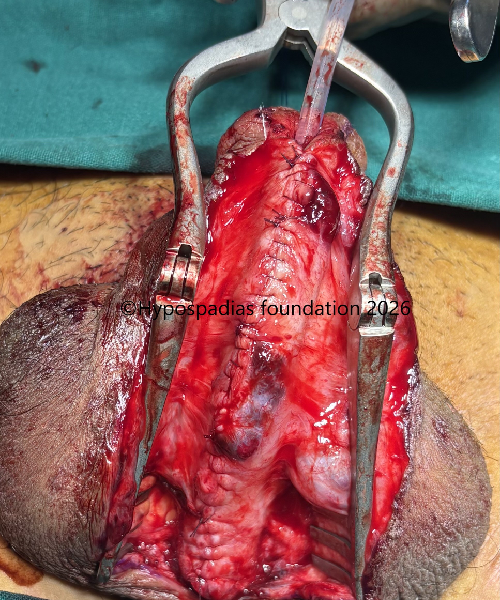
Fig 13: Graft edges incised and deepened till the corpora. First layer of urethroplasty done in continuous subcuticular fashion with 5-0 vicryl over 12Fr silicone catheter. Second layer closed with local tissues with 5-0 vicryl.
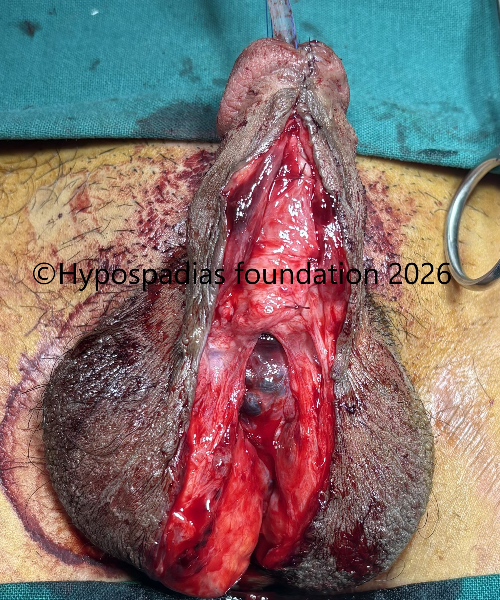
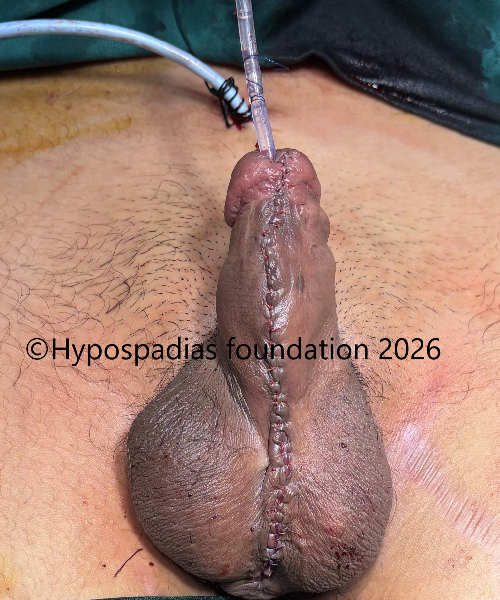
Fig 14: Dartos tissue mobilized on either side and sutured over the urethroplasty with 5-0 vicryl. Skin closed with 5-0 vicryl. Suprapubic catheter placed at the end of the procedure.
Single-Stage Repair of Proximal Penile Hypospadias with Split Preputial Onlay Flap Urethroplasty
Proximal Penile Hypospadias is a congenital condition in which the urethral opening (meatus) is in the proximal penile region rather than at the tip of the glans. Surgical management involves correction of penile curvature (chordee correction) and reconstruction of the urethra to bring the urinary opening to the tip of the penis. Early surgical correction is important to preserve normal urinary function and future sexual function.
Most pediatric urologists and hypospadias surgeons prefer a two-stage repair for proximal penile hypospadias, particularly in cases where:
1. Chordee is significant
2. The urethral plate is narrow or of poor quality
3. A long segment urethral reconstruction is required
Management of complex failed hypospadias Staged Reconstruction in an 11- Year-Old Boy
The current case was a complex failed hypospadias as the patient developed multiple persistent complications following previous surgeries. This patient had a combination of issues rather than a single complication, such as urethral stricture and residual or recurrent chordee (penile curvature), poor cosmetic outcome and scarred, fibrotic penile tissues.
Patients with failed or multiple-repair hypospadias commonly present with poor urinary stream or spraying, dysuria (painful urination), recurrent urinary tract infections (UTIs), urine leakage from multiple fistula sites, residual penile curvature, urethral stones or obstructive symptoms and severely scarred, irregular penile skin and/or glans deformity. The penile tissues in these cases are usually fibrotic and scarred, poorly vascularized and unsuitable for primary reconstruction.
Management of complex severe hypospadias almost always requires a staged reconstructive approach, typically performed in 2 to 3 stages, depending on tissue quality and skin availability. In stage 1, excision of scarred and fibrotic tissues, correction of chordee, reconstruction of penile skin is performed. Placement of oral mucosa graft (OMG) is commonly required and done in stage 2 and urethroplasty in stage 3. Also, in cases with severe skin shortage, a three-stage repair is preferred to ensure safe and tension-free reconstruction.
Oral mucosa graft has become the gold standard in complex redo hypospadias surgery because it is resistant to wet environment, has excellent vascular integration, shows good long-term durability and is ideal when local penile tissues are scarred or unusable. In complex redo cases, postoperative hyperbaric oxygen therapy (HBOT) is often used to improve tissue oxygenation, enhance graft survival, promote wound healing and reduce risk of complications.
Management of failed hypospadias cases requires a high level of surgical expertise due to multiple previous failed surgeries, scarred and distorted anatomy and high risk of complications. Such cases should ideally be managed in specialized hypospadias centers with experience in complex and redo urethral reconstruction.
About Hypospadias Foundation
The Hypospadias Foundation is a dedicated center for the treatment of children and adults with hypospadias and complex genital reconstruction. The foundation provides personalized care for patients from India and more than 30 countries worldwide. It is located at MITR Hospital, Navi Mumbai where more than 250 hypospadias surgeries are performed annually.
Dr A K Singal is senior hypospadias and reconstructive urologist with extensive experience in primary and failed hypospadias surgery. Dr Singal is rated as the best hypospadias surgeon in India and the world. Dr Ashwitha Shenoy is a specialist in pediatric urology with focused interest in hypospadias reconstruction. Their combined expertise has contributed to high success rates in complex redo hypospadias cases
