Failed hypospadias with urethral stricture and fistula – Two stage oral mucosa graft urethroplasty
A 6-year male child presented to Hypospadias foundation OPD after 4 failed hypospadias surgeries in Australia. After the first surgery in Australia, he had complete breakdown of the newly reconstructed urethra. He further underwent redo surgery in 3 stages, but it was unsuccessful. Even after a redo surgery, child was unable to pass the urine from the distal penile meatus. On examination in the Hypospadias Foundation OPD, the urinary opening was at the midpenile region. The distal passage was completely strictured. There was no obvious chordee on examination. We counselled the parents that the entire repair needs to be done again in 2-3 stages.
At the start of hypospadias surgery, we performed cystoscopy. The urethra proximal to the midpenile meatus was normal. Scope could not be negotiated into the distal urethra. Chordee was assessed and there was no residual chordee. We decided to proceed with two stage oral mucosa graft repair since there was no residual chordee.
Glans stitch was taken with 4-0 prolene. The distal urethra was laid open and noted to be completely stenosed. Unhealthy fibrotic urethra was excised completely. Oral mucosa graft was harvested from the right cheek of size 5x2cm. Graft was placed on the ventral raw area and quilted thoroughly on the corpora with 6-0 PDS.
After stage 1, healing was good. Steroid massage was started 3 weeks after surgery and was continued for 5 months. There was 100% graft uptake. Second surgery was planned 8 months after stage 1 when graft was soft and pliable.
Second stage repair (Urethroplasty)
Local anesthesia, lignocaine with adrenaline was injected at the edges of the graft. Graft was incised at the margin keeping a width of 18mm. Graft was tubularized over a 7Fr infant feeding tube (IFT). Second layer was closed with local tissues. Glans wings were widely mobilized. Dartos flap was raised from the left side and sutured over the urethroplasty with 6-0 PDS. Glansplasty was done with 5-0 vicryl and glans epithelium was closed with 6-0 PDS. Skin was closed in 2 layers with 6-0 PDS and 6-0 vicry rapide.
Dressing change was done on day 7 and catheter was removed on post operative day 12. After catheter removal, the child was passing urine in single straight stream with no pain or leak.
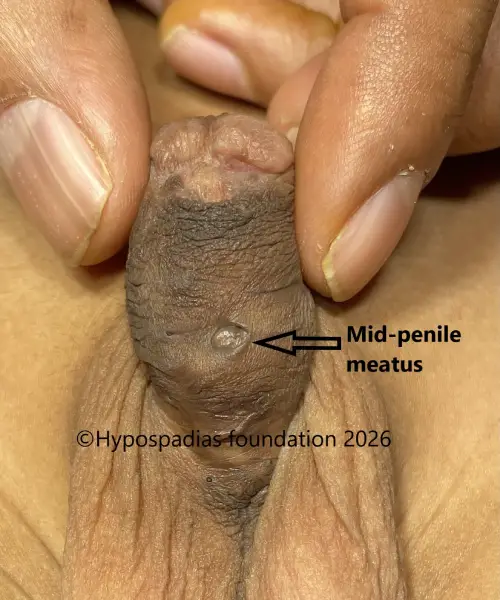
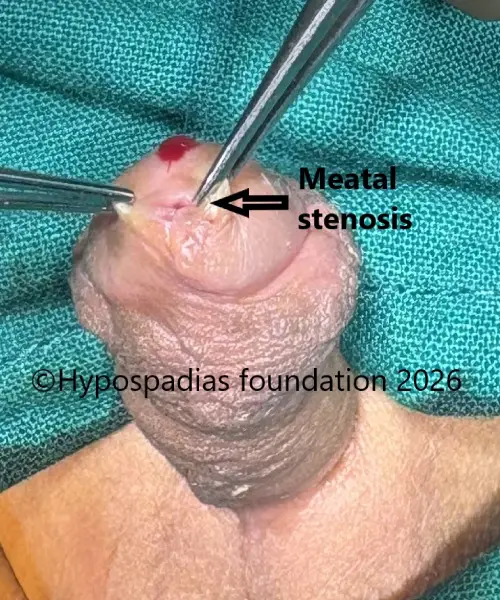
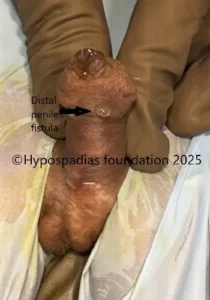
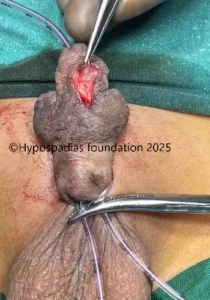
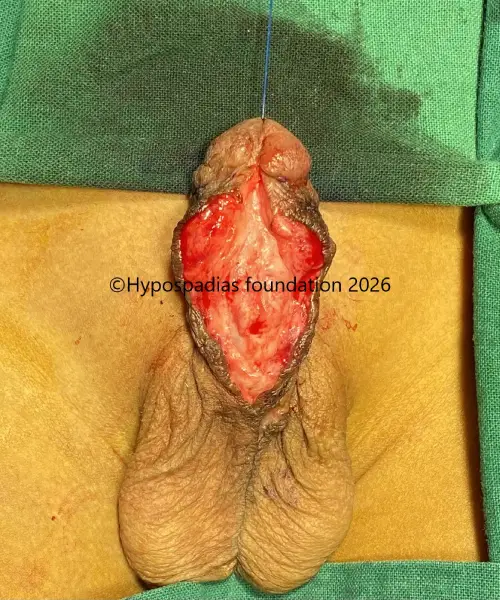
Picture 1: On examination, the meatus was in the midpenile region. Chordee was assessed during stage 1, there was no residual chordee

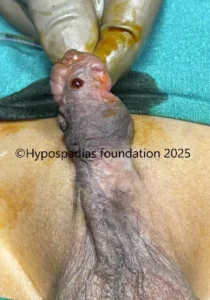
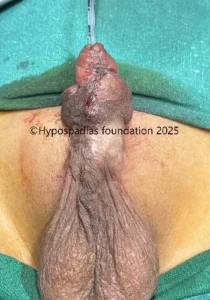
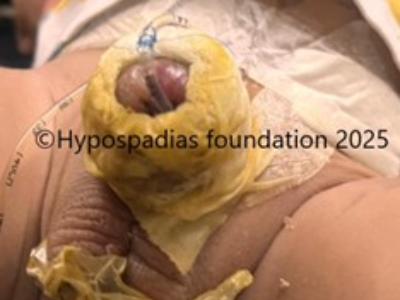
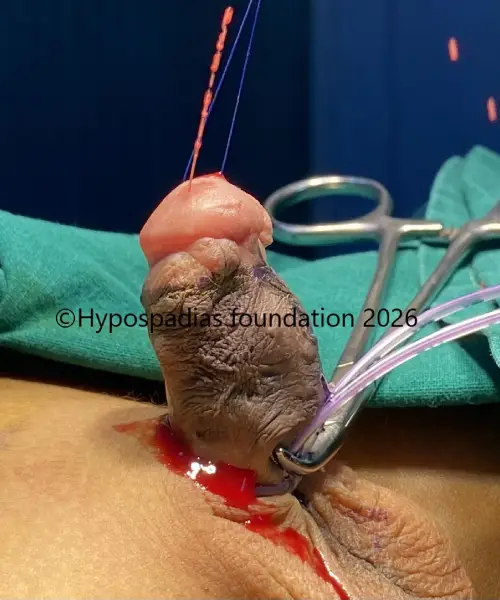
Picture 2: Pre surgery urine stream, passing urine from midpenile region with no flow from the distal penile meatus.
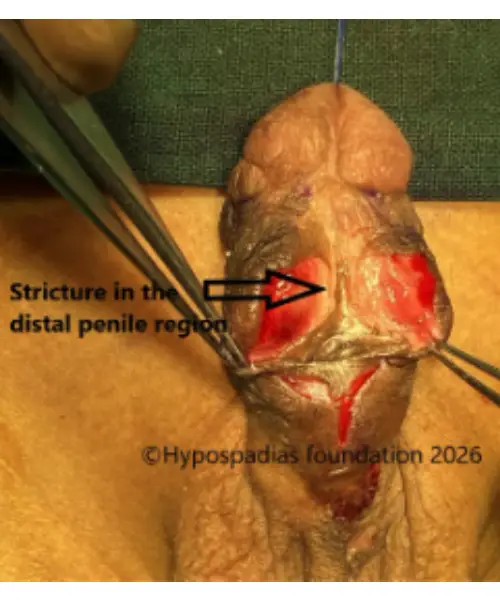
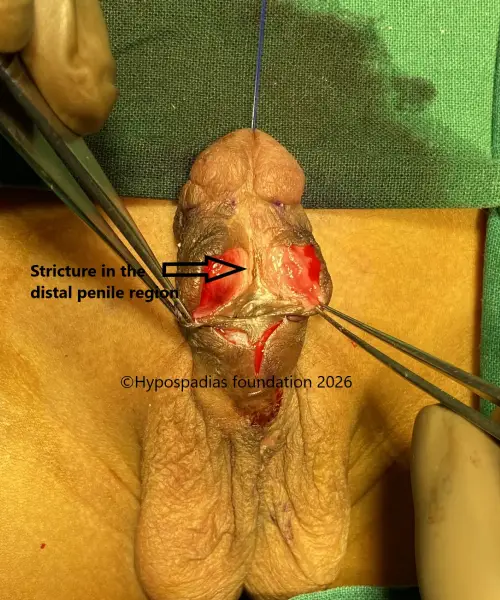
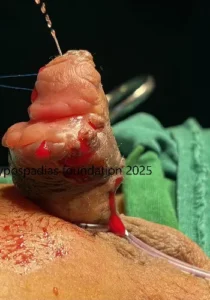
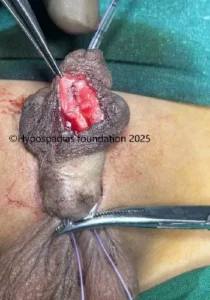
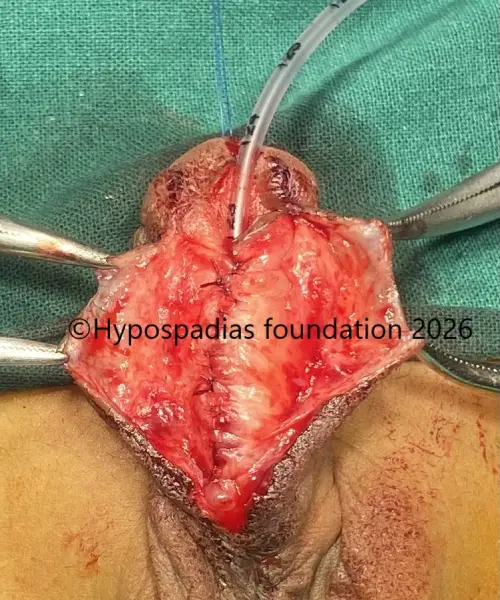
Picture 3: Distal urethra was laid open and noted to be completely stenosed.
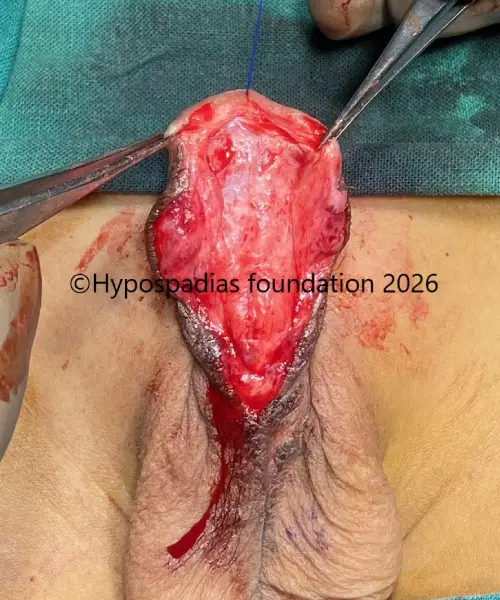
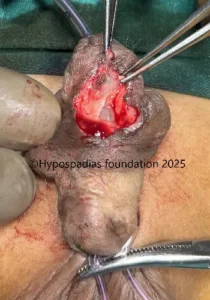
Picture 4: Unhealthy urethra excised, glans wings widely raised for placement of oral mucosa graft
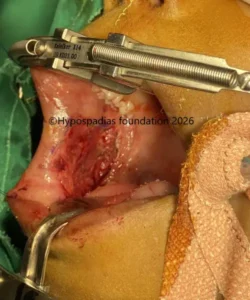
Picture 5: Oral mucosa graft harvested from right cheek, sutured on the ventral side and quilted to the underlying corpora with 6-0 PDS.
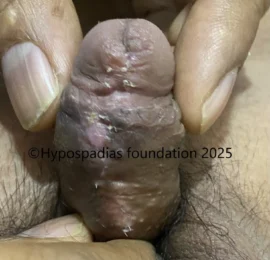

Picture 6: At 3 weeks after stage 1 OMG, the graft was examined. There was 100% graft uptake
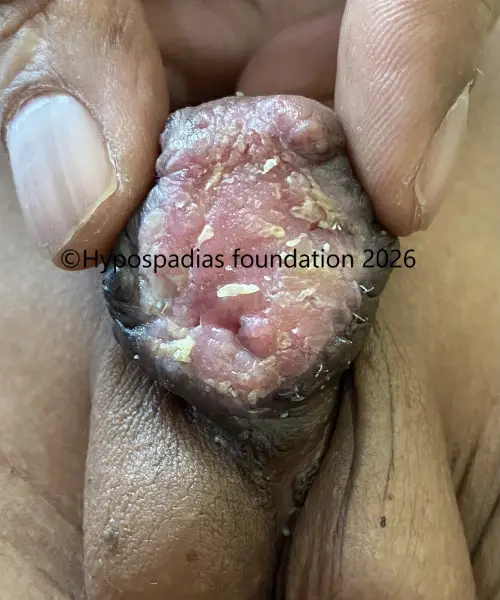
Picture 6: Follow up at 6 months after surgery
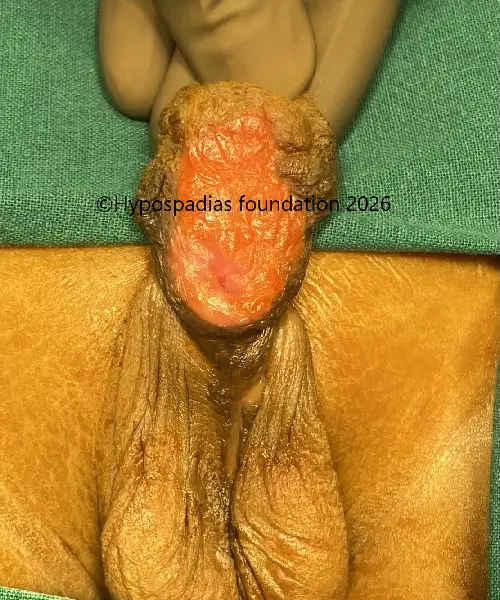
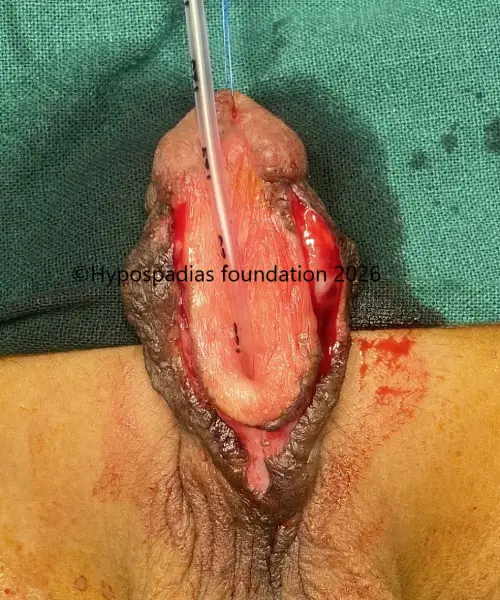
Picture 7: Graft was soft and supple at 8 months after stage 1. Graft edges were incised keeping a width of 18mm for urethroplasty
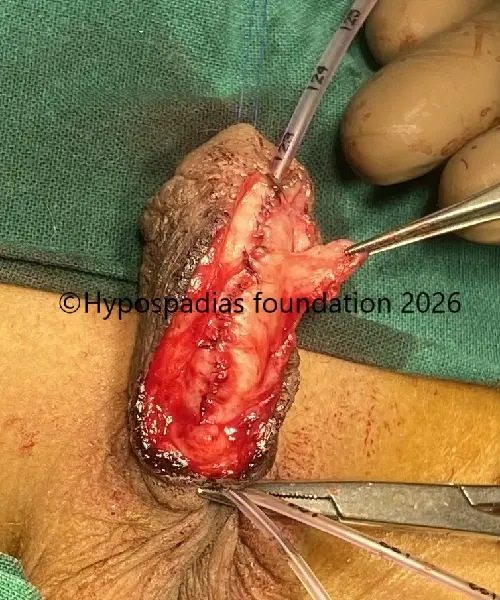
Picture 8: Urethroplasty was done over 7Fr infant feeding tube. Dartos flap from the left side was raised and sutured over the urethroplasty.
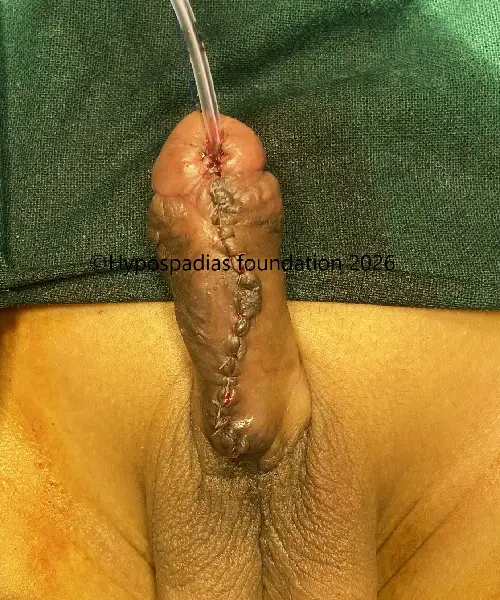
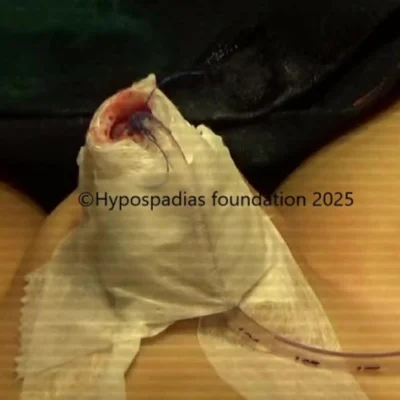
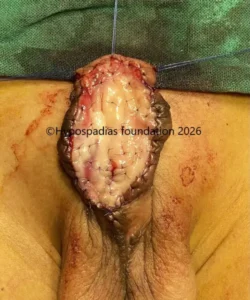
Picture 9: Urethroplasty and glansplasty was completed. Catheter removal was done on post operative day 12
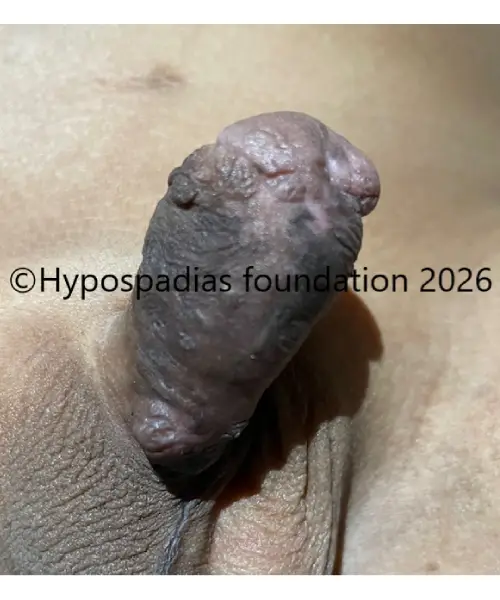

Picture 10: Cosmetic result and urine stream at 6 months after stage 2 urethroplasty
Surgery for failed hypospadias – stricture and fistula – Two stage oral mucosa graft repair
Failed hypospadias with stricture and fistula – Two stage oral mucosa graft urethroplasty
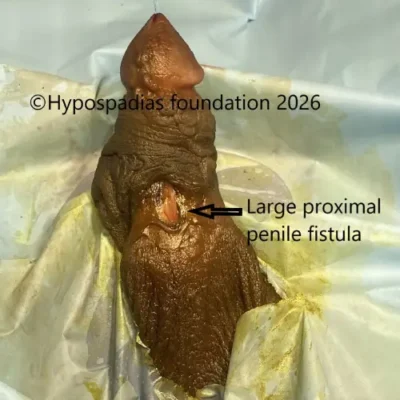
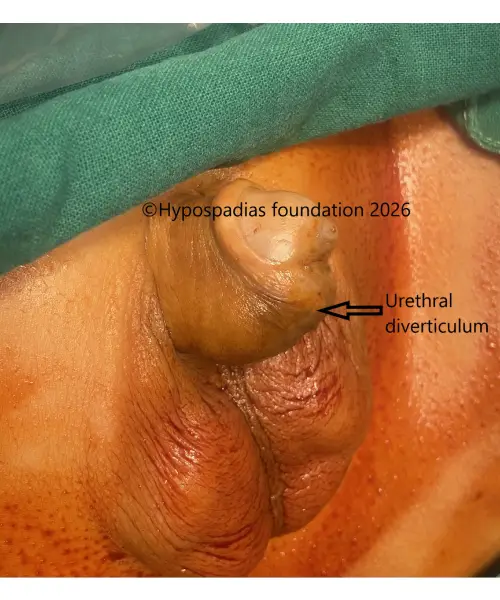
Urethral stricture and urethrocutaneous fistula are two well-recognized complications following hypospadias repair. A urethral stricture refers to narrowing of the reconstructed urethra due to scarring. This obstruction is one of the important factors contributing to fistula
formation.
In the above-mentioned case, the child developed distal urethral narrowing and was unable to pass urine through the distal penile meatus. As a result, the urethra opened in the mid- penile region, allowing urine to drain from the bladder. Since urine preferentially drained through the mid-penile opening, flow across the distal urethra ceased, leading to progressive stenosis of the distal segment. Over time, this resulted in narrowing of the entire distal urethra.
The most common causes of urethral stricture following hypospadias surgery include ischemia of the neourethra due to poor vascularity, excessive tension on the reconstructed urethra, and postoperative infection. Urethral strictures occurring after hypospadias repair differ significantly from non-hypospadias–related urethral strictures. In such cases, urethral dilatation is usually ineffective, and repeated dilatations may further worsen the scarring and narrowing.
Management of post-hypospadias urethral stricture typically requires replacement of the narrowed segment with healthy tissue. This is achieved using either oral mucosal grafts (such as buccal mucosa) or well-vascularized local skin flaps to adequately widen the urethra and restore normal urinary flow.
Complications following hypospadias repair are best managed by a trained and experienced pediatric urologist, particularly one with expertise in failed and complex hypospadias cases. Multiple previous surgeries significantly increase the complexity of subsequent repairs. In such situations, staged surgical reconstruction often provides better functional outcomes, improved cosmesis, and more durable long-term results.
At the Hypospadias Foundation India, children and adults from more than 30 countries worldwide seek treatment for hypospadias and its complications. The surgical team, led by experienced surgeons Dr. A. K. Singal and Dr. Ashwitha Shenoy, specializes in managing complex, multistage, and failed hypospadias repairs. Dr A.K.Singal is considered the best hypospadias surgeon in the world especially for children or adults who had a failed hypospadias surgery earlier. With a deep understanding of the nuances involved in challenging hypospadias surgery, the Hypospadias Foundation offers a dedicated and specialized approach for patients requiring advanced reconstructive care.