25-year-old adult presented to the Hypospadias Foundation OPD with complaints of severe curvature of the penis. There were no urinary complaints. He also that the curvature has worsened over time. On examination, there was severe ventral curvature (downward bending) of the penis. Meatus was located on the glans and was normal in location. No plaques were felt on palpation. Ultrasound doppler of the penis was done which was normal. He was counselled for surgery. Surgery was planned in single or two stage depending on the degree of curvature and the ventral urethral calibre.

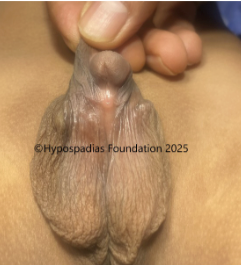
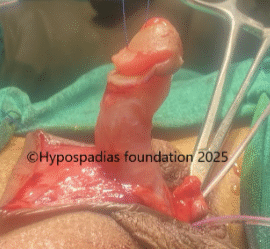
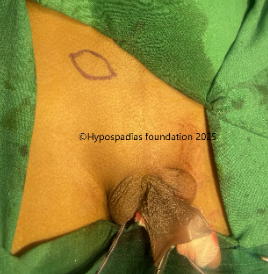
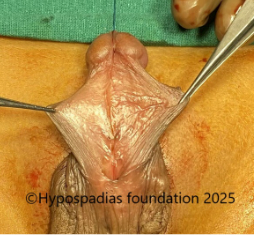
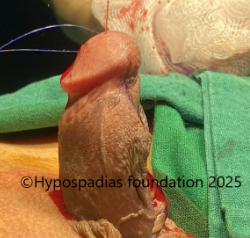
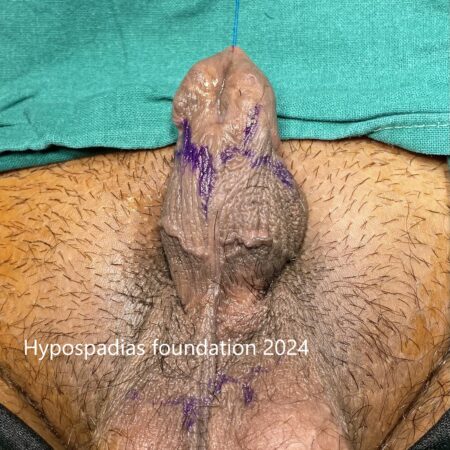
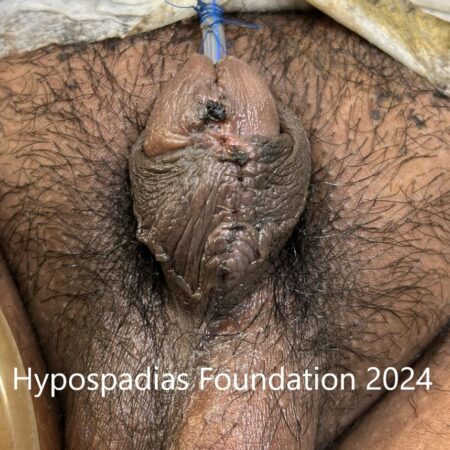
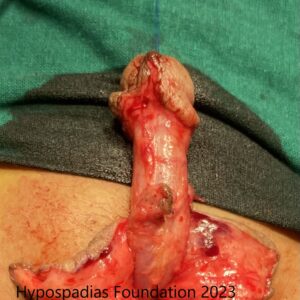
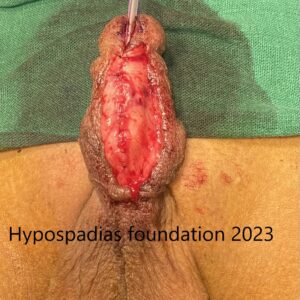
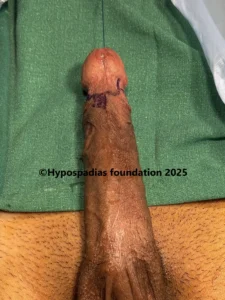
Picture 1: Severe curvature of the penis noted on erection
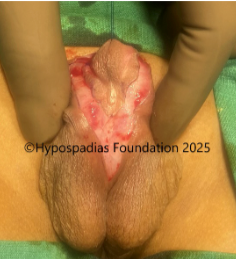
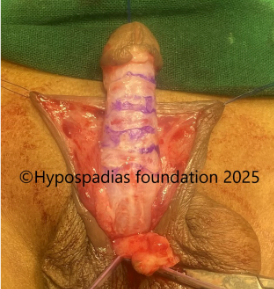
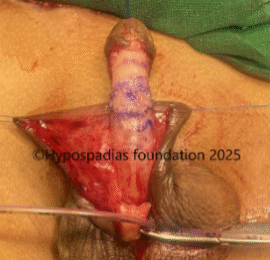
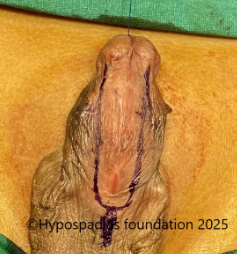
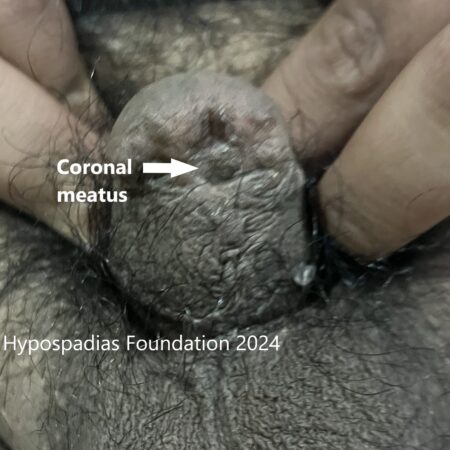
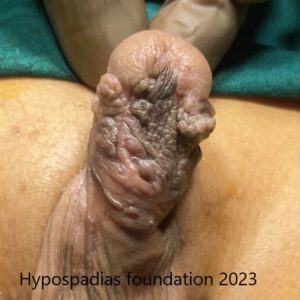
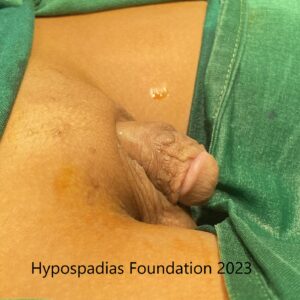
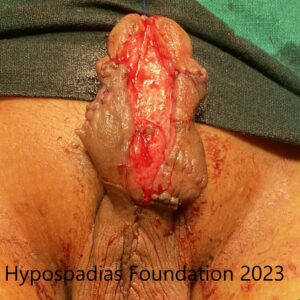
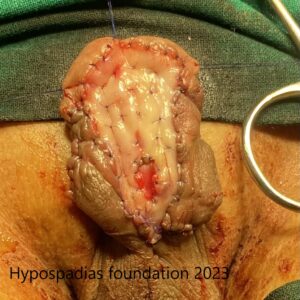
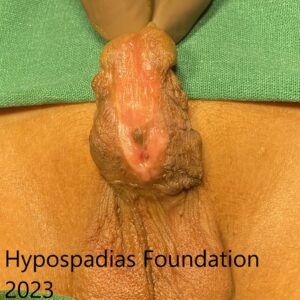
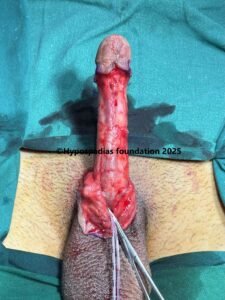
Picture 2: Pre-operative assessment showed normal location of the meatus. Second image shows marking for degloving
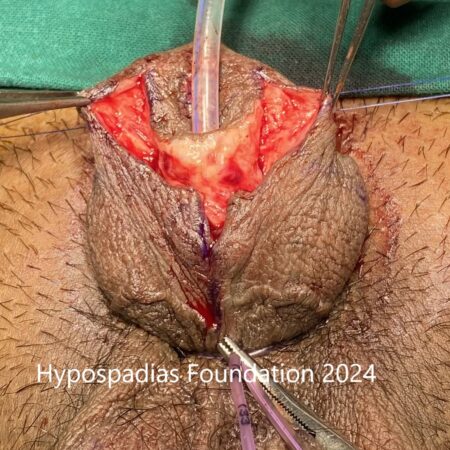
Surgery was started by taking a stay stitch on the glans with 4-0 prolene. Marking of the incision was done and local anaesthesia lignocaine with adrenaline was injected at the marked site. Complete degloving was done. Chordee was assessed by artificial erection test and more than 60-degree chordee was noted. Since the penile length was good and urethra was not appearing short or taut, we decided to proceed with dorsal plication procedure to correct the chordee.
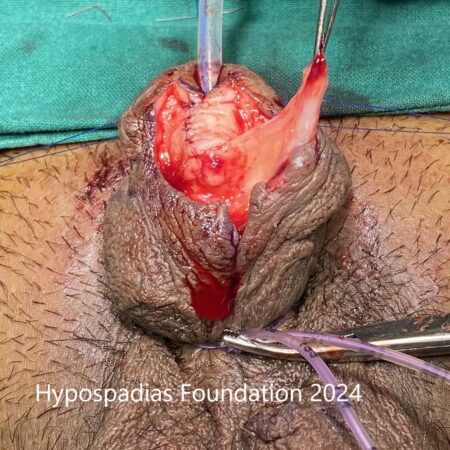
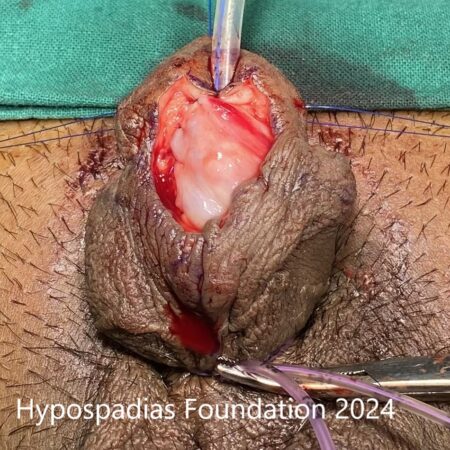
Buck’s fascia along with neurovascular bundle was raised on the dorsal side starting laterally and upto the midline. Chordee was reassessed and exact site of curvature was marked. 24 dots(12 dots on either side) were marked. 4 dots proximal and 8 dots distal to the site of maximum curvature. Longitudinal plication sutures were placed at these sites with 4-0 prolene involving full thickness tunica albuginea. Chordee was reassessed and there was no chordee. Chordee was completely corrected by these plication sutures. Buck’s fascia was closed on either side with 6-0 PDS. Circumcision was completed and skin rearranged and closed in 2 layers with 6-0 PDS and 5-0 vicryl rapide. 12Fr silicone catheter was placed per urethra and dressing was done. Catheter was removed after 7 days. Follow up at 6 months after surgery, there was no chordee and the erection was straight.
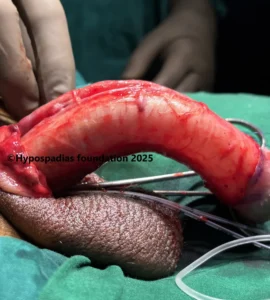
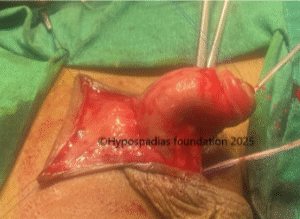
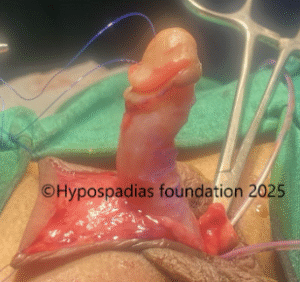
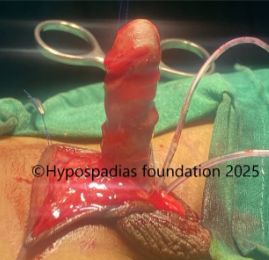
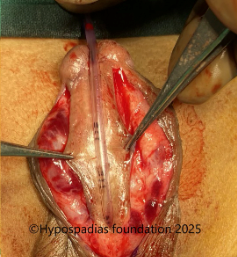
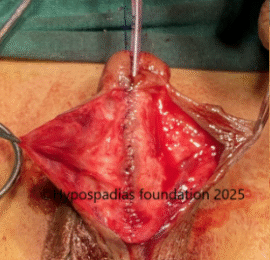
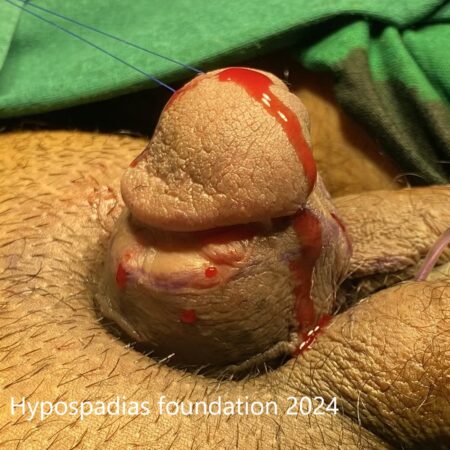
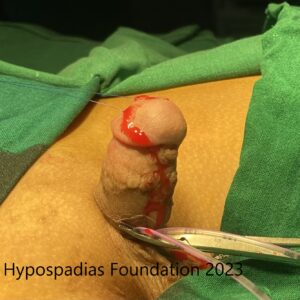
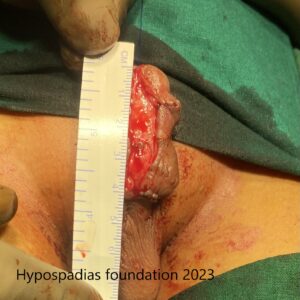
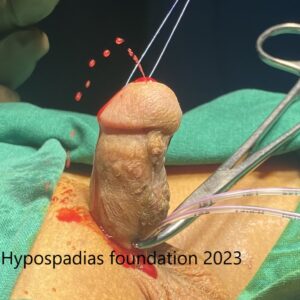
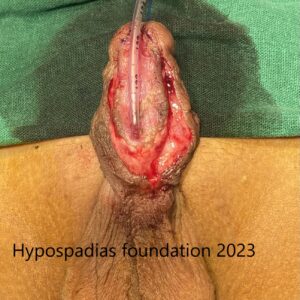
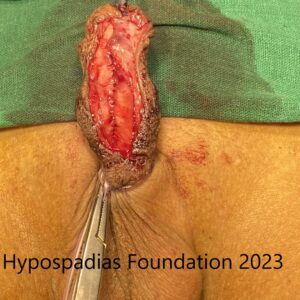
Picture 3: Complete degloving done and artificial erection test done which showed more than 60-degree chordee.
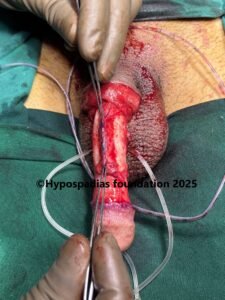
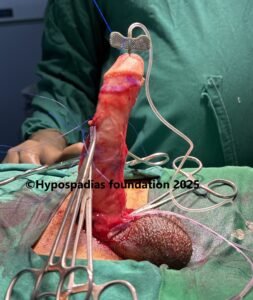
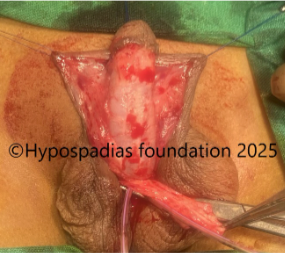
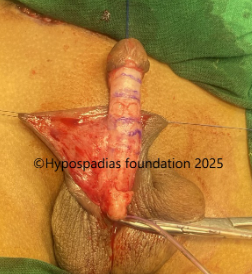
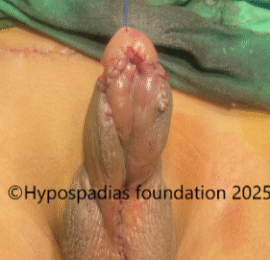
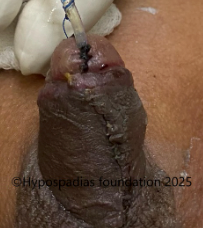
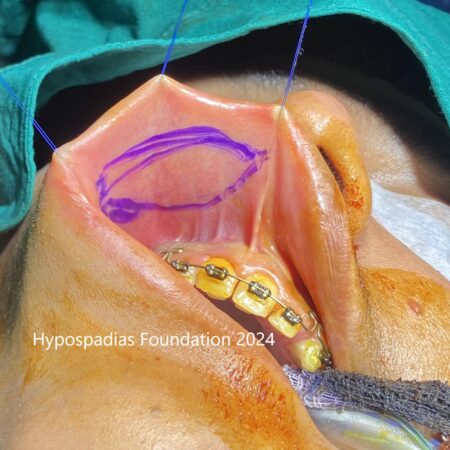
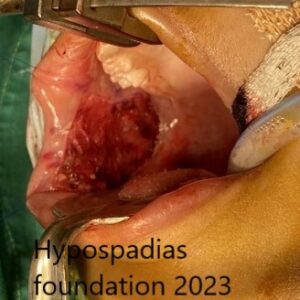
Picture 4: Neurovascular bundle raised on both sides upto the midline. Marking done, plications sutures placed, held and artificial erection test done. No chordee noted
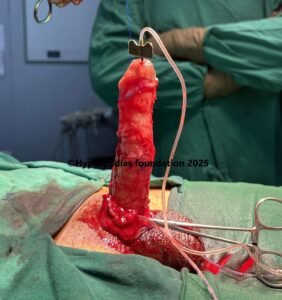
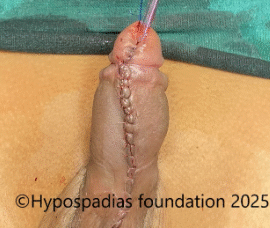
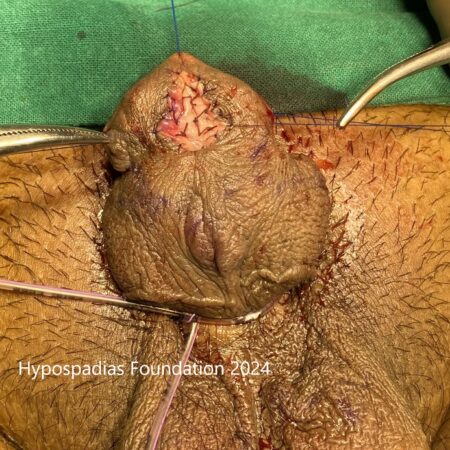
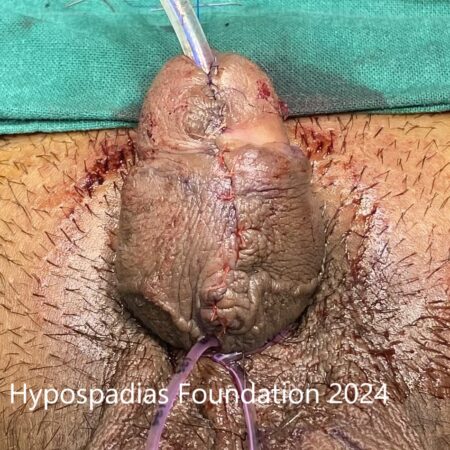
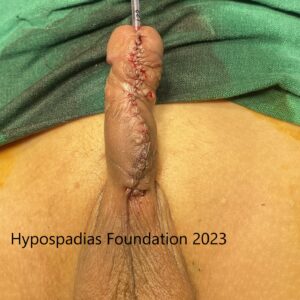
Picture 5: 24 dot plication completed and circumcision done

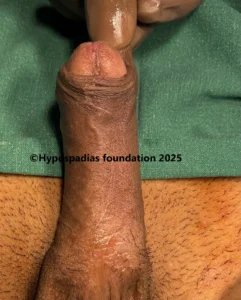
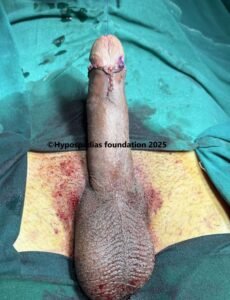
Picture 6: Penile erection straight 6 months after surgery
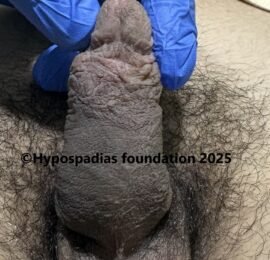
Picture 7: Cosmetic result 6 months after surgery
Severe ventral chordee in adults: Diagnosis and management
Chordee is characterized by curvature of the penis which is noticeable only during penile erection. This is congenital (present at birth) but can be missed in childhood and can present with challenges in adulthood potentially causing discomfort, affecting sexual function and can also have psychological implications impacting self-esteem.
In chordee, there is noticeable bend in the penis during an erection which can be downward, upward or sideways. It can cause pain or discomfort during erection or sexual intercourse. Surgical correction is the only effective method of chordee correction in adults. The goal of the surgery is to straighten the penis and restore normal function. Chordee correction can be done by dorsal plication or ventral lengthening procedure. Ventral lengthening procedure is done if there is short urethra which contributes to the penile curvature. If the urethra is normal with good penile length, then dorsal plications are preferred.
In the above-mentioned case, the penile length was good, and the urethra was normal hence we proceeded with dorsal plication. In this procedure multiple (16 or 24) non absorbable fine sutures are strategically placed on the convex side of the penis. These sutures are placed in pairs and in parallel fashion to create plications in the tunica albuginea. Neurovascular bundles are carefully raised before placing the plication sutures.
Important note for adult chordee
It is essential for adults considering chordee correction to have a thorough evaluation by a hypospadias specialist who specialized in penile reconstructive surgery. The surgeon will assess the type and degree of curvature, discuss the case and recommend the most appropriate surgical technique whether plication or a staged procedure.
At hypospadias foundation, we get adults and children from all over the world in search of treatment for hypospadias. We provide support and information for children, adults and their families affected by hypospadias. Dr Singal and Dr Shenoy are deeply devoted to creating awareness and helping patients get the right treatment for hypospadias be it primary, redo or adult hypospadias. Children and adults from more than 25 countries visit our hypospadias foundation in search for cure and are cured of hypospadias.
Dr A K Singal is a highly experienced surgeon and regarded as the best hypospadias surgeon in India and in the world. He has dedicated his life towards treating children and adults with hypospadias. His expertise in this area has helped us achieve excellent outcomes in adults and children with hypospadias.
Dr Ashwitha Shenoy is an expert pediatric surgeon with special interest in pediatric urology and hypospadias. Both Dr Singal and Dr Shenoy work together to give