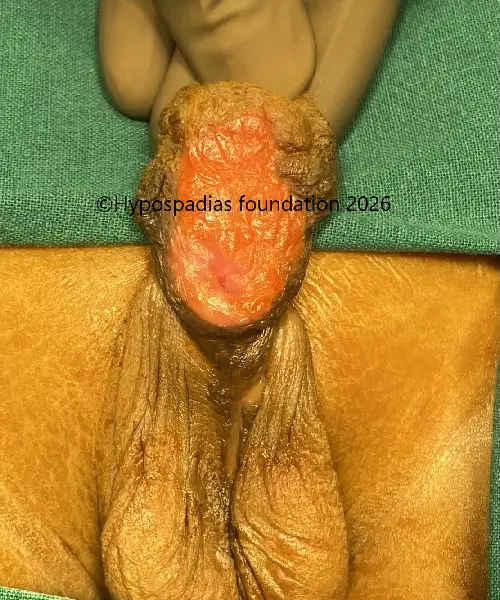
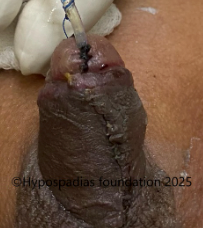
Mast A.T., a one-year-old male, presented to the Hypospadias Foundation clinic with an abnormal ventral urinary opening on underside of penis and downward penile curvature. Clinical examination revealed a distal penile hypospadias, deficient ventral foreskin, and
ventral chordee (penile curvature).
A single-stage surgical hypospadias repair was planned, comprising of chordee correction (Orthoplasty) and urethroplasty (reconstruction of the urinary channel)
Intraoperative Procedure
The procedure commenced with a 5-0 Prolene stay suture on the glans for traction. Local anaesthesia (Xylocaine with adrenaline) was infiltrated at the marked incision sites. Following the initial incision and complete degloving of the penis, an artificial erection test was performed to assess the degree of curvature.
Chordee Correction: A curvature of less than 30 degree was noted. This was corrected via Tunica Albuginea Plication (TAP) on the dorsal aspect (upper part) of the penis, opposite the site of maximum curvature. A repeat artificial erection test confirmed complete correction of the chordee.
Urethroplasty: The glans wings were marked, incised, and widely mobilized. A midline incision was made in the urethral plate to increase its width (TIP – Tubularized Incised Plate technique). The neo-urethra was constructed in two layers:
o Layer 1: Continuous subcuticular sutures.
o Layer 2: Interrupted sutures.
Waterproofing: A preputial dartos flap was raised and transposed over the urethroplasty site to provide a vascularized waterproofing layer, significantly reducing the risk of a fistula (leak).
Completion: Glansplasty was performed to reconstruct the glans. The skin was closed in two layers using 6-0 PDS and 6-0 vicryl Rapide.
Postoperative Outcome and Follow-up
The repair was stented using a 7 Fr infant feeding tube, with the new meatus successfully positioned at the tip of the glans.
Day 7: The catheter and dressings were removed. The patient demonstrated a strong, straight urinary stream with no associated pain.
Healing: The surgical site healed by primary intention without complications (e.g., hematoma, infection, or dehiscence).
1-Year Follow-up: The patient remains asymptomatic with excellent functional and cosmetic results.

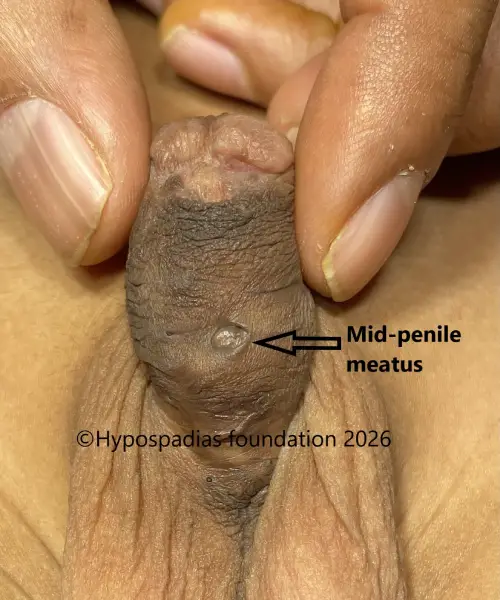
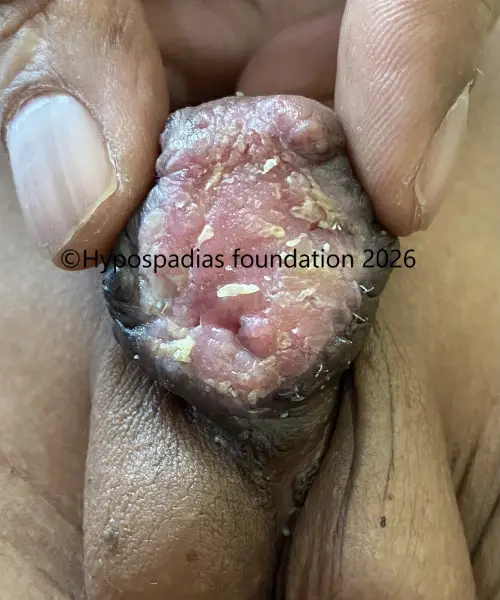
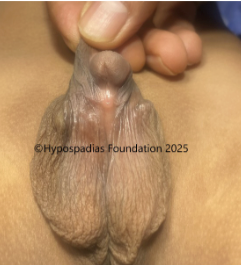
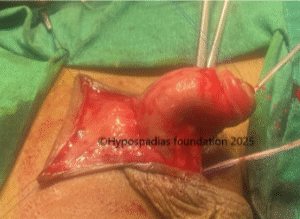
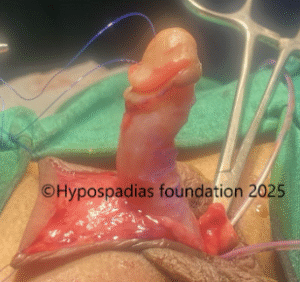
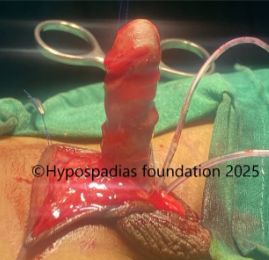
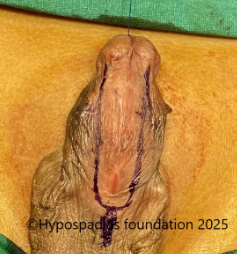
Pic 1: Clinical examination shows presence of chordee with meatus in the distal penile region
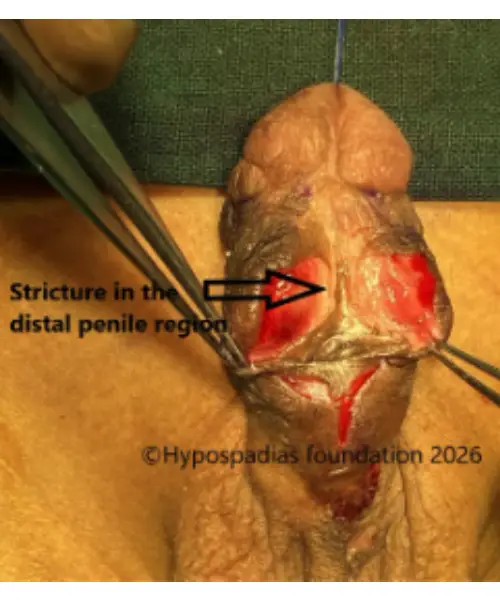
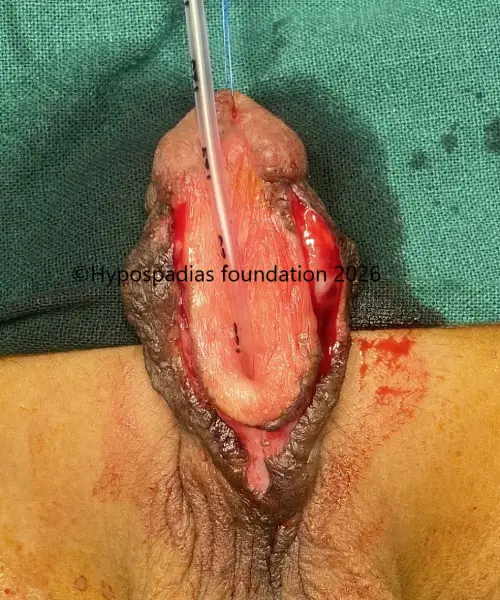
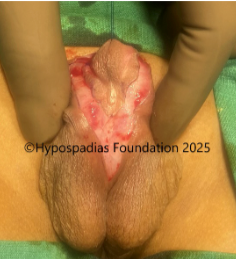
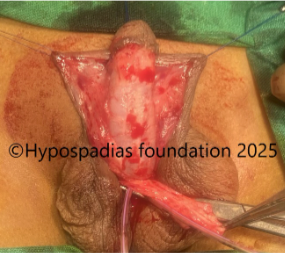
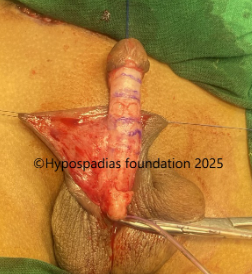
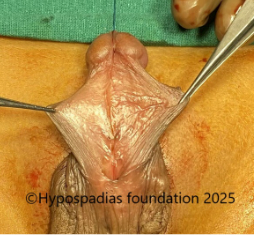
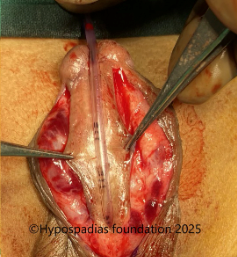
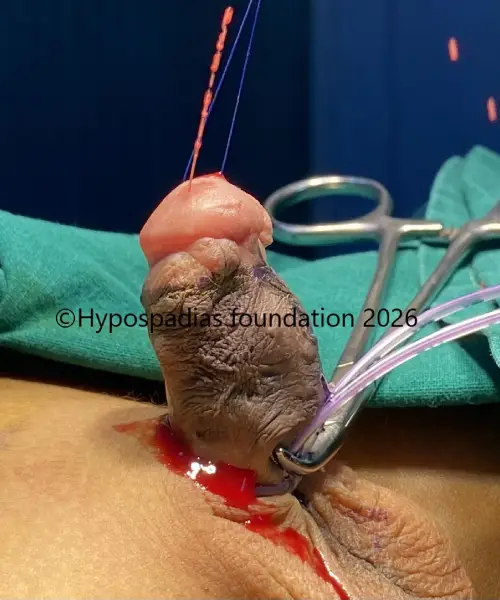
Pic 2: Complete degloving done
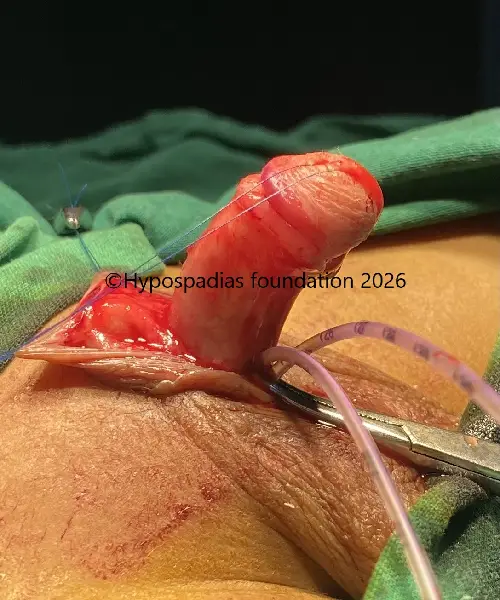
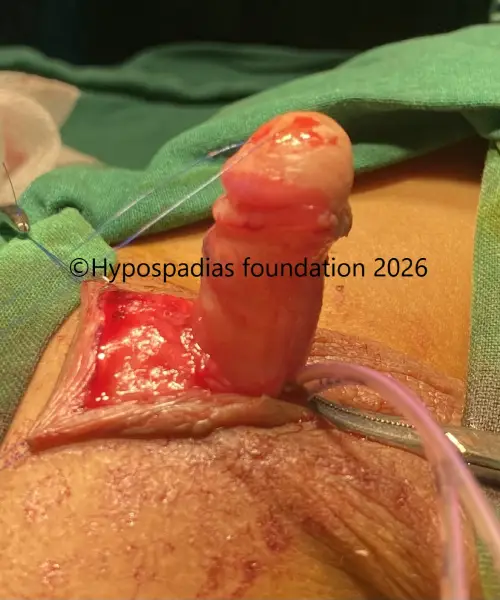
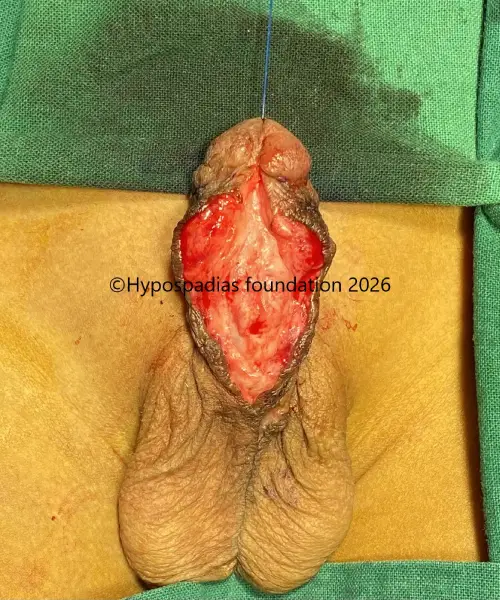
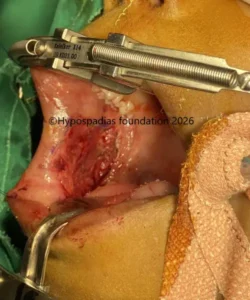
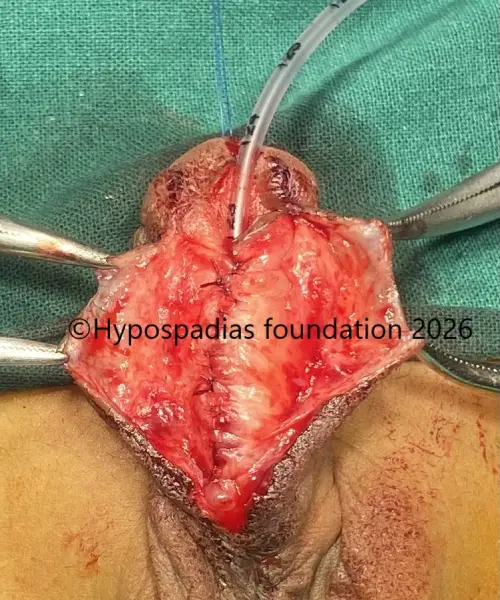
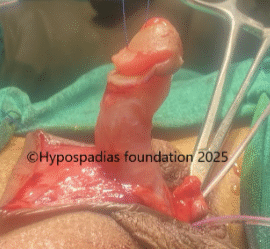
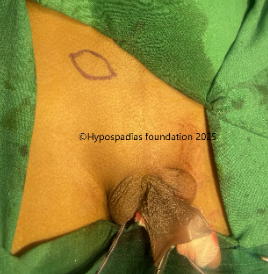
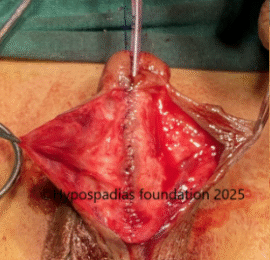
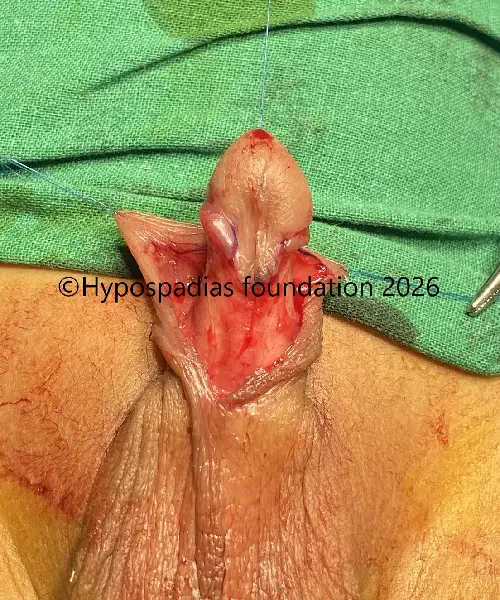
Fig 3: Artificial erection test shows less than 30-degree chordee which was corrected by 12’o clock dorsal tunica albuginea plication (dorsal TAP)
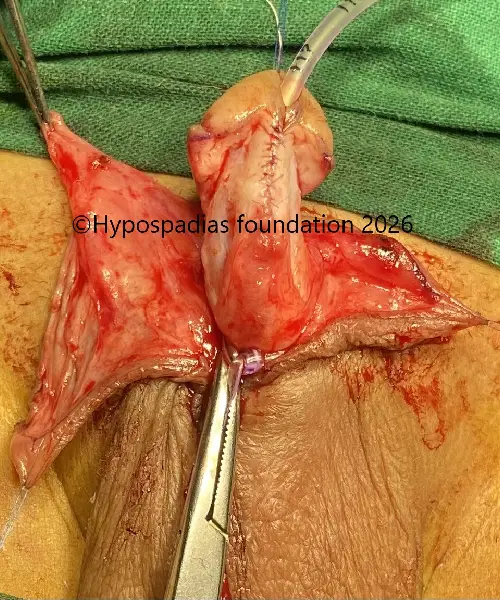
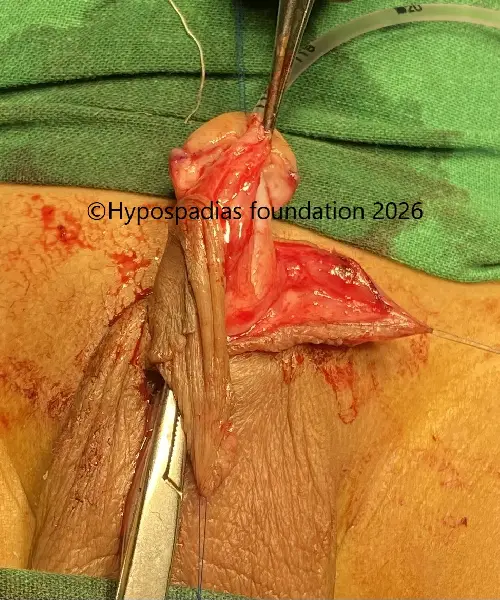
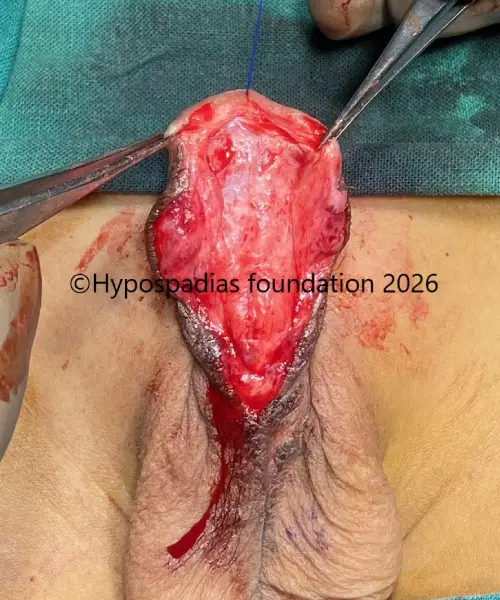
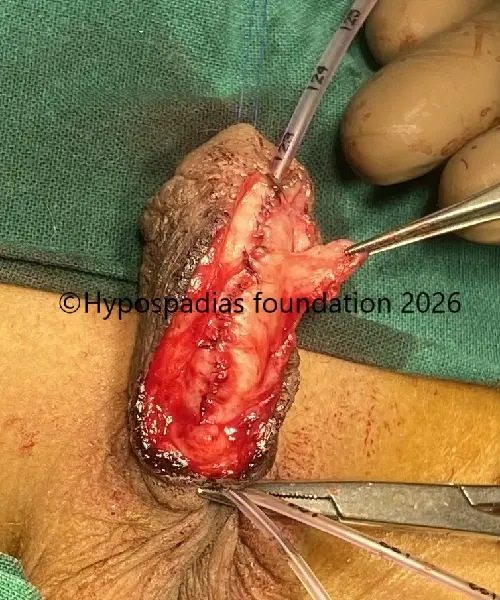
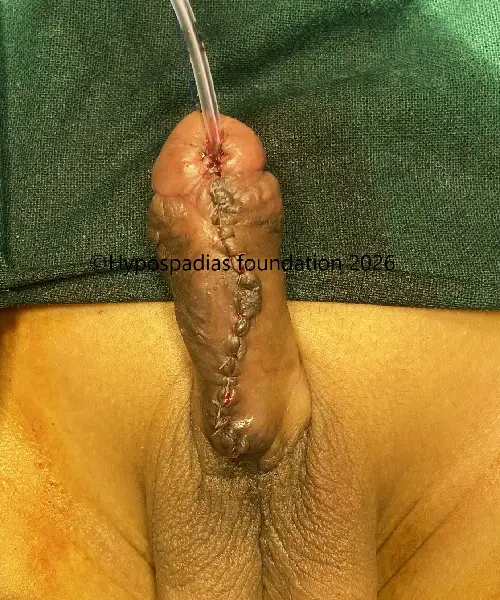
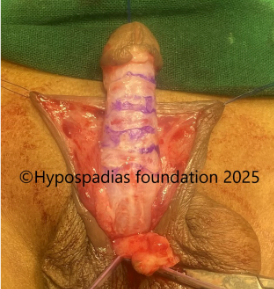
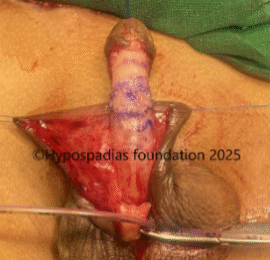
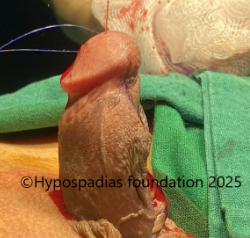
Fig 4: Glans wings raised and urethroplasty done over 7Fr infant feeding tube. Right dartos flap raised and sutured over the urethroplasty with 6-0 PDS.
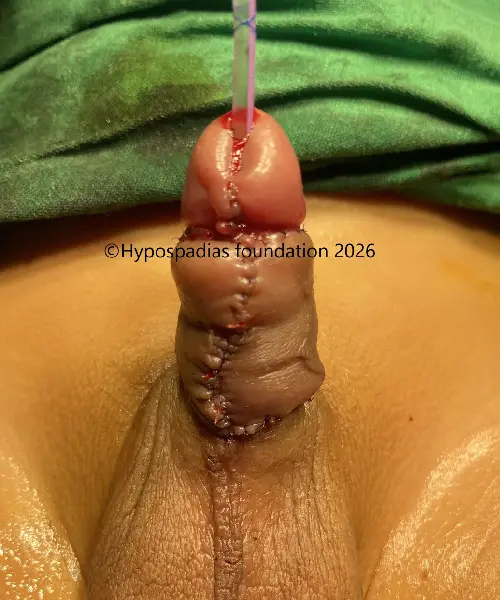
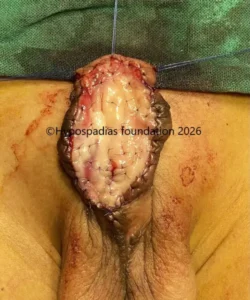
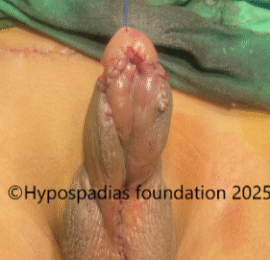
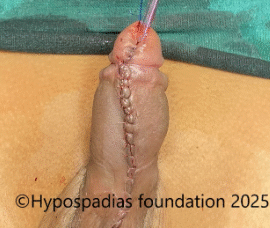
Fig 5: Single stage urethroplasty with chordee correction completed
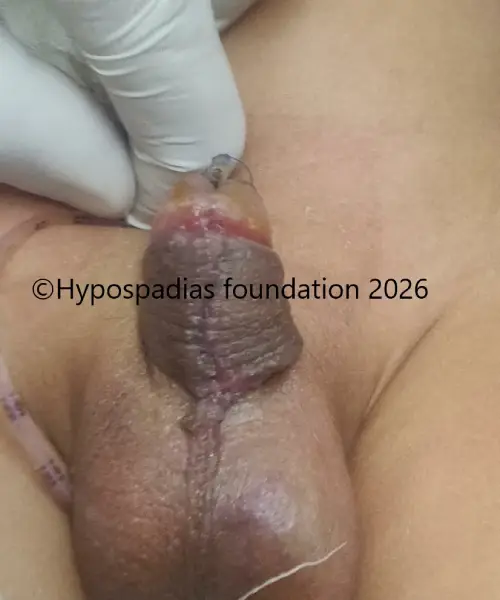
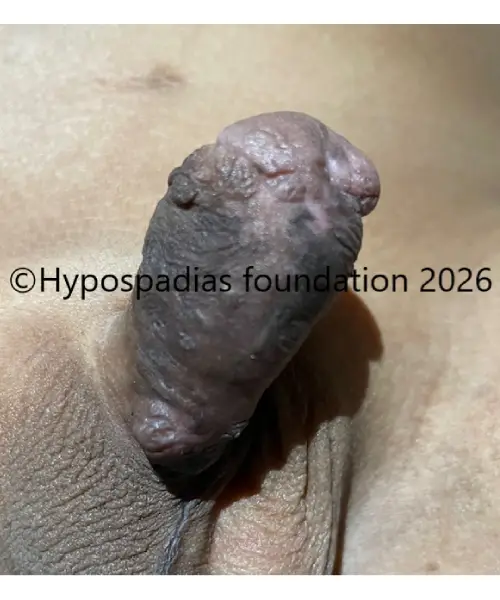
Fig 6: At 7 days follow up after surgery

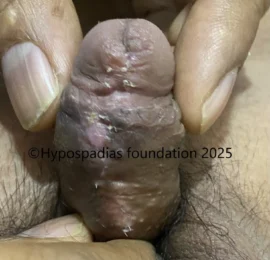
Fig 7: At 1 year follow up after surgery, passing urine in single straight stream
Single-stage hypospadias repair in distal penile hypospadias with chordee Single-stage hypospadias repair is the preferred surgery for distal penile hypospadias associated with mild chordee. Though the urinary opening is positioned near the glans, the reconstruction has to be done with utmost care by the hypospadias expert.Even a little bit of carelessness can lead to complications.
Primary Technique: The Tubularized Incised Plate (TIP) urethroplasty—commonly referred to as the Snodgrass repair—is the most widely utilized method. This procedure involves a midline incision of the urethral plate to allow for tension-free tubularization, ensuring a functional and cosmetically normal neo-urethra.
Optimal Age for Surgery: Pediatric urologists generally recommend performing this repair between 6 and 18 months of age. This "golden window" facilitates rapid tissue healing, simplifies postoperative diaper management, and minimizes the risk of long- term psychological impact on the child.
Outcomes and Success Rates
When performed by an expert hypospadias surgeon in a specialized center like Hypospadias Foundation India, the success rate for distal repairs exceeds 95%. However, clinical diligence is required to monitor for potential postoperative hypospadias complications.
Functional Rationale for Early Surgical Intervention
While distal hypospadias may appear manageable in infancy, untreated cases often lead to significant functional and psychosocial challenges as the patient matures:
1. Backward flow of urine: If the urinary opening is located on the underside of the penis, the stream is directed backwards causing inconvenience to the boys. Boys will have difficulty in using a urinal and they cannot urinate without getting urine on their clothes or shoes.
2. Sexual Health: Persistent chordee (ventral curvature) can lead to painful erections or Mechanical difficulties with intercourse in adulthood.
3. Psychosocial Impact: A non-apical urinary opening can cause significant social anxiety and hygiene concerns regarding standing to void.
Clinical Summary: Early repair of distal hypospadias with chordee is not merely cosmetic; it is a functional necessity that ensures optimal urogenital health and quality of life into adulthood.
The Hypospadias Foundation: A Global Center of Excellence
Located in Kharghar, Navi Mumbai, Maharashtra, the Hypospadias Foundation stands as India’s premier and best hypospadias specialty center and a globally recognized leader in hypospadias treatment.
Why Patients Choose Our Center:
For over 18 years, we have been a destination for both pediatric and adult patients from across India and the world. Our commitment to surgical precision and patient care is reflected in our clinical data:
High Volume: Over 250 specialized surgeries performed annually.
Proven Safety: A complication rate of less than 5%, significantly lower than the global average for complex reconstructions.
Global Reach: Successfully treating international patients from more than 30 countries with diverse anatomical challenges.
Our Expert Surgical Team
The foundation’s success is built on the combined expertise of two of the world’s leading specialists in reconstructive urology.
Dr A. K. Singal is a top-tier expert hypospadias surgeon and pediatric urologist who has dedicated his career to the advancement of hypospadias repair. His refined techniques have consistently achieved excellent functional and aesthetic outcomes for both children and adults, particularly in complex "redo" or failed previous surgeries. He is rated the best hypospadias surgeon in India and the world.
Dr Ashwitha Shenoy is an expert pediatric urologist with a sub-specialty interest in pediatric urology and hypospadias. Her meticulous approach to neonatal and childhood reconstruction ensures long-term success from a young age. Together, Dr. Singal and Dr. Shenoy provide a collaborative, multidisciplinary approach that delivers the best results for hypospadias surgery in India.