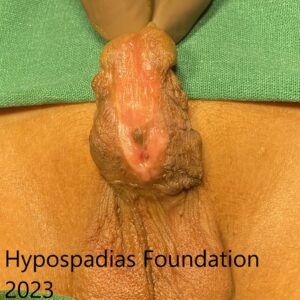
A 3 year 6 months male child presented to us in the OPD after two failed surgeries for hypospadias (done elsewhere). He had undergone a staged hypospadias repair at another centre in Mumbai and when he came to us, he had meatus at the proximal penile region probably due to complete dehiscence after stage 2 repair. The child was very apprehensive in the OPD because of a traumatic experience from previous surgery. On examination, the meatus was in the proximal penile region with very irregular unhealthy skin beyond that. At our centre, he was planned for cystoscopy, chordee assessment and most likely a staged oral mucosa graft hypospadias repair for best outcome.
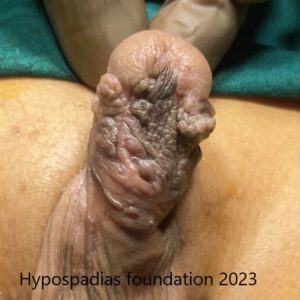
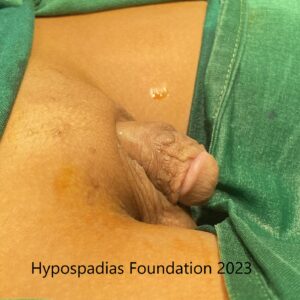
On clinical examination, the meatus was at the proximal penile region with
unhealthy distal skin.
At the start of hypospadias surgery, chordee was assessed and there was no residual chordee noted. Deep degloving was done, all fibrotic tissues from the urethral bed were removed. Proximal urethra was mobilized. Chordee was reassessed and no chordee was noted. Skin was rearranged on the dorsal and ventral side. Raw area of 4x2cm was noted on the ventral aspect. Hence, we planned a stage 1 OMG repair i.e placement of oral mucosa graft.
Oral mucosa graft was harvested from the right cheek and placed on the ventral side from the glans till the meatus. Graft was quilted thoroughly on the corpora using 6-0 PDS.
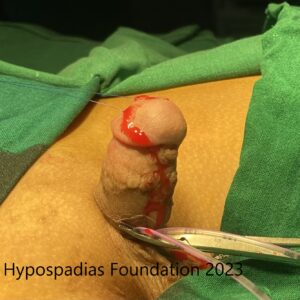
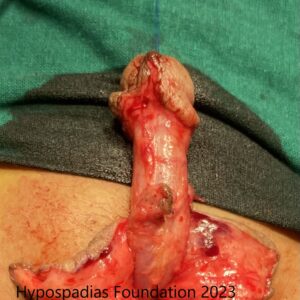
Chordee was assessed, no residual chordee noted. Deep degloving done, all fibrotic tissues excised.
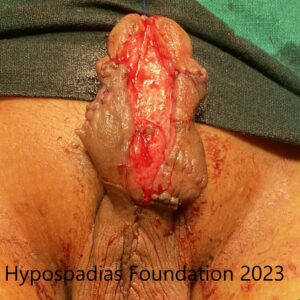
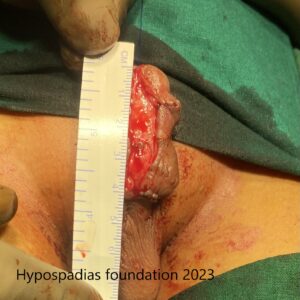
Skin rearranged on the dorsal and ventral side. 4cm raw area on the ventral side noted.
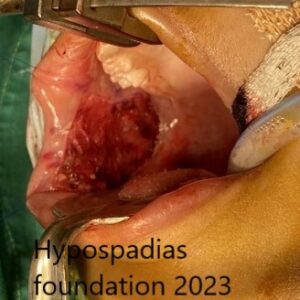
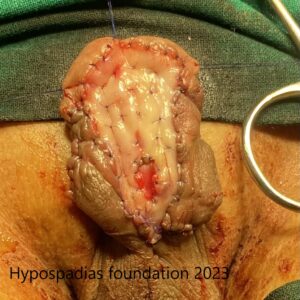
Oral mucosa graft harvested from the right cheek of size 4x2cm. Oral mucosa graft sutured on the ventral side from the glans till all around the meatus.
After stage 1, graft healing was good. Steroid massage was started 3 weeks after surgery and was continued for 5 months. Graft uptake was 100%. Second stage was planned after 6 months when the graft was soft and pliable. During the second stage hypospadias repair, chordee was reassessed and no chordee noted. Local anaesthesia – lignocaine with adrenaline was injected at the edges of the graft. Graft was incised at the margins and tubularized over a 7Fr Infant feeding tube (IFT). Second layer was closed using local tissues. Dartos flap was harvested from the left side and sutured over the urethroplasty using 6-0 PDS. Glans wings were widely mobilized and Glansplasty was done using 6-0 PDS. Glans epithelium was closed using 6-0 PDS. Skin was closed in 2 layers using 6-0 PDS and 6-0 vicryl rapide.
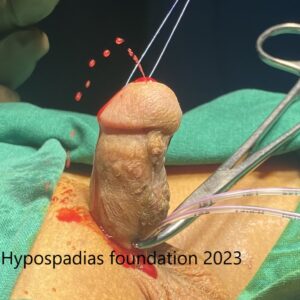
Graft was soft, 6 months after stage 1 repair. Chordee was assessed and no chordee was noted.
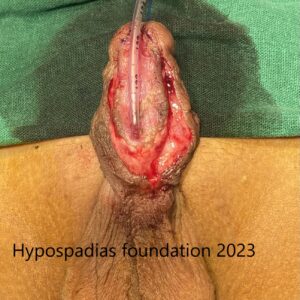
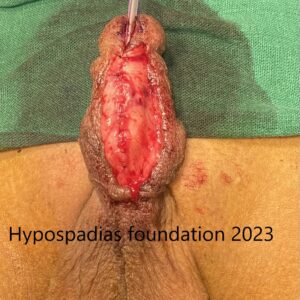
Graft was measured and 18mm width was used for urethroplasty. Graft was incised all around and tubularized and sutured using continuous inverting subcuticular sutures using 6-0 PDS.
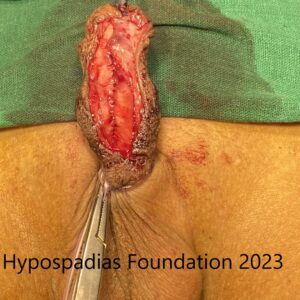
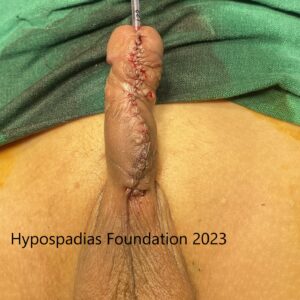
Dartos flap sutured over the urethroplasty. Glansplasty and skin done hence completing Stage 2 OMG urethroplasty.
Dressing change was done after 7 days, and catheter was removed after 10 days. After catheter removal, the child passed urine in single straight stream with no pain or leak.

Post catheter removal, passing urine in single straight stream with no complications.
Two stage oral mucosa graft repair in redo hypospadias
Hypospadias is usually diagnosed after birth in the neonatal period by a pediatrician. Once diagnosed, referral to a pediatric urologist is necessary to plan surgery at the right age. As per the guidelines the best age for hypospadias surgery is between 9 to 18 months. Hypospadias Surgery is planned in single or two stages depending on the severity of hypospadias. After chordee correction, usually there is insufficient skin on the underside of the penis to reconstruct the urethra hence extra tissues either in the form of prepuce (in primary ones) and oral mucosa graft (in redo cases) are used for urethroplasty.
Prepucial skin can be mostly used only once for the hypospadias repair. If the first surgery is unsuccessful then we need to plan redo surgery by using skin from somewhere else due to lack of local prepucial skin. In these children, use of oral mucosa graft is an excellent option. The reason why oral mucosa can be used for urethral reconstruction is because it is hairless, thin and pliable similar to the natural lining of the urethra. Graft is harvested from the inside of the cheek or lip, fatty tissue from the graft is removed. The penis is prepared for placement of the graft and the graft is meticulously sutured on the corporal bed. The graft incorporates into the urethral bed and becomes soft in 6-8 months. Local Steroid massage is necessary to make the graft soft. Once it is as soft as lip it can be tubularized to form the neourethra. The beauty of oral graft is such that there is less risk of fistula formation, minimal donor site scarring and has good cosmetic outcomes. However, it requires specialized skill and experience to perform oral mucosa graft in hypospadias and there is a small percentage of adults or children who may develop graft rejection or failure. In these children or adults, we need to replace the graft completely by a new graft.
The above-mentioned case is of a boy who presented to us after two failed hypospadias surgeries in the past. The local prepucial skin was unhealthy, hence we opted for oral mucosa graft. The final cosmetic result in this boy was excellent and he was able to pass urine in single straight stream with no complications.
At Hypospadias Foundation in Navi Mumbai, after hypospadias repair including oral mucosa inlay graft urethroplasty, children are encouraged to walk, play, and do some activities at home comfortably. We do not advice bed rest. Tying the legs and restricting children from doing activities or walking is disturbing for the child. Encouraging them to do activities can act as a distraction and take their mind off from the discomfort and promote healing. With our vast experience in hypospadias, we would recommend that children be allowed to do some activities in the post operative period. Play can be powerful tool for children to express their emotions and process surgical fear.
About Hypospadias foundation
Hypospadias foundation is an organization dedicated for children and adults with hypospadias and is rated as the best hospital for hypospadias repair in India. It was founded in 2008 by Dr A K Singal and is located in Kharghar, Navi Mumbai. Hypospadias foundation offers best results for surgical repair for primary and failed hypospadias. We at hypospadias foundation believe in providing personalized care and psychosocial support to families of children and adults with hypospadias. The foundation also advocates improved access of care for people with hypospadias around the world.
Dr A K Singal is a well renowned hypospadias surgeon and regarded as the best hypospadias surgeon in India and in the world. His vision for hypospadias has helped him achieve excellent outcomes in adults and children with hypospadias. He has dedicated his life in treating children and adults with hypospadias with his innovative surgical techniques.
Dr Ashwitha Shenoy is an expert pediatric surgeon with special interest in pediatric urology and hypospadias. She holds a particular interest in hypospadias and along with Dr Singal performs advanced surgical techniques for both primary and complex hypospadias cases in children and adults.
Contact us:
For appointment kindly contact us at the contact details given below.
MITR hospital & Hypospadias Foundation, Kharghar, Navi Mumbai, India – Tue/Saturday 4:00pm-6:00pm, Call for appointments: +91-9324180553. Or email us at hypospadiasfoundationindia@gmail.com
or pls call up our clinic for an appointment – +91-9324180553

