A 2-year-2-month-old male child presented to the Hypospadias Foundation clinic with the complaint of passing urine from the penoscrotal region since birth. On clinical evaluation in the outpatient department, the child was noted to have moderate chordee with the urethral meatus located in the penoscrotal region, consistent with Severe Hypospadias. On genital examination, the penile size was small, with a stretched penile length (SPL) of 25 mm and glans diameter (GD) of 10 mm.
Given the small penile size, an hCG stimulation test was performed to evaluate the underlying hormonal status. The test demonstrated a good increase in testosterone levels following hCG administration, but insufficient conversion of testosterone to dihydrotestosterone (DHT), suggesting impaired androgen conversion. This was suggestive of 5 Alpha reductase deficiency.
Based on these findings, the child was started on topical Dihydrotestosterone (DHT) gel therapy. The treatment was continued for two months. Following DHT gel application, there was a significant improvement in penile size, with the glans diameter increasing to 15 mm. After discontinuation of DHT therapy, hypospadias repair surgery was planned two months later to allow stabilization of local tissue effects.
Post-therapy examination revealed improvement in penile size, and the urethral meatus appeared to be located in the proximal penile region rather than the penoscrotal region.
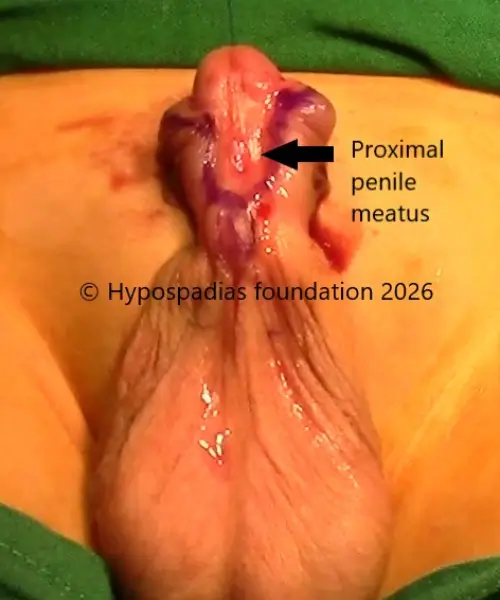
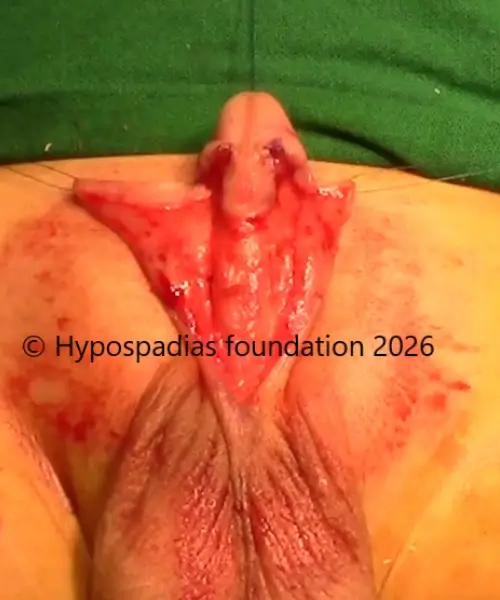
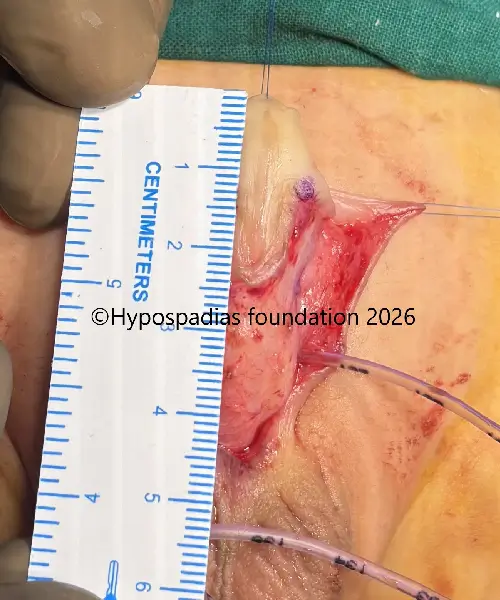
Pic 1: Clinical examination in the operation theatre showed proximal penile meatus. Complete degloving done.
Operative Procedure
The surgery was initiated by placing a stay suture on the glans using 5-0 Prolene suture. The degloving incision was marked, and local anesthesia with Lignocaine and adrenaline was infiltrated along the marked incision line. A deep penile degloving was performed. Following degloving, chordee assessment was carried out using the Artificial Erection Test. The curvature was measured and noted to be less than 30°. Correction of the chordee was achieved using 12-o’clock dorsal Tunica Albuginea Plication (TAP). After plication, the artificial erection test was repeated and no residual chordee was observed.
Given the intraoperative findings, a single-stage repair was planned. As the case involved a long urethroplasty segment with a narrow urethral plate and a flat glans, a modified Preputial Onlay Flap Repair was selected. This technique is particularly suitable for hypospadias with mild chordee which is correctable without division of urethral plate, narrow urethral plate, and shallow or flat glans.
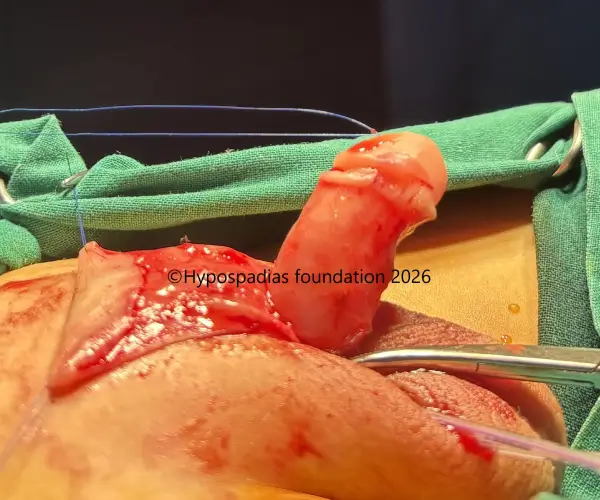
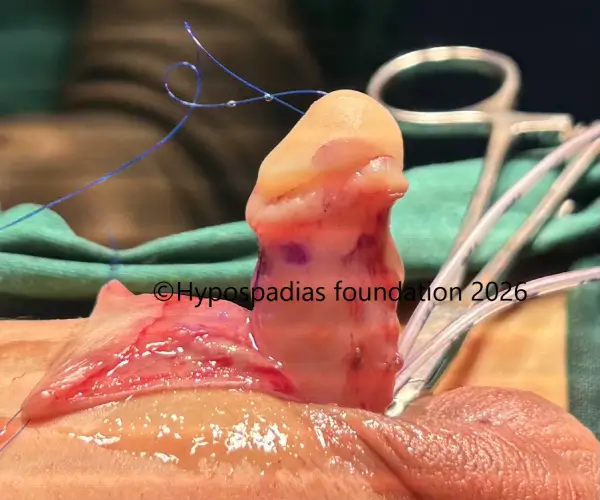
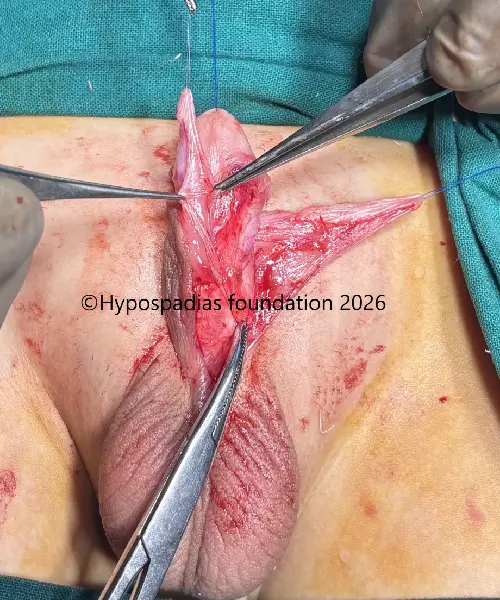
Pic 2: An Artificial Erection Test was performed to assess penile curvature. A mild distal chordee of less than 30° was noted. Chordee correction was carried out using 12-o’clock dorsal Tunica Albuginea Plication. Following plication, the artificial erection test was repeated and no residual chordee was observed.
The required flap length was measured. The dorsal prepuce was divided in the midline, and the right half of the prepuce was used to raise the onlay flap. A stay suture using 6-0 PDS suture was placed at the edge of the flap for traction. The flap width was maintained at approximately 6 mm. The flap, along with the underlying dartos tissue, was carefully mobilized until the desired reach was obtained. A midline relaxing incision was made in the urethral plate to widen it. Urethroplasty was then initiated by placing three interrupted sutures at the proximal end of the repair at the 7, 6, and 5 o’clock positions. This was followed by a continuous edge-to-edge anastomosis between the preputial onlay flap and the margins of the urethral plate, completing the urethral reconstruction.
Pic 3: The required length of flap was measured and split prepucial flap was raised with good dartos tissue
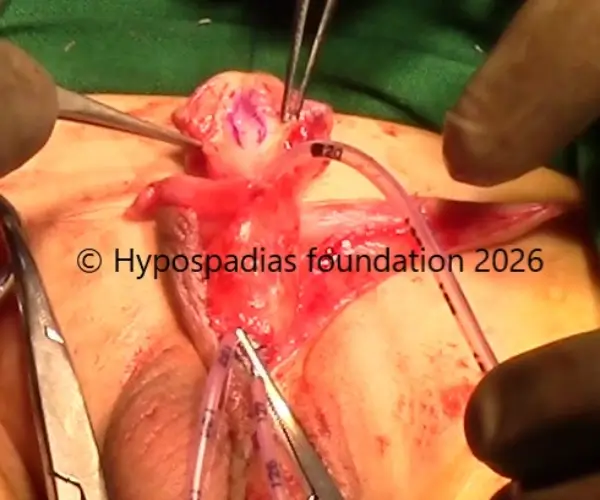
Fig 4: Glans wings raised and urethroplasty done over 7Fr infant feeding tube. Right dartos flap raised and sutured over the urethroplasty with 6-0 PDS.
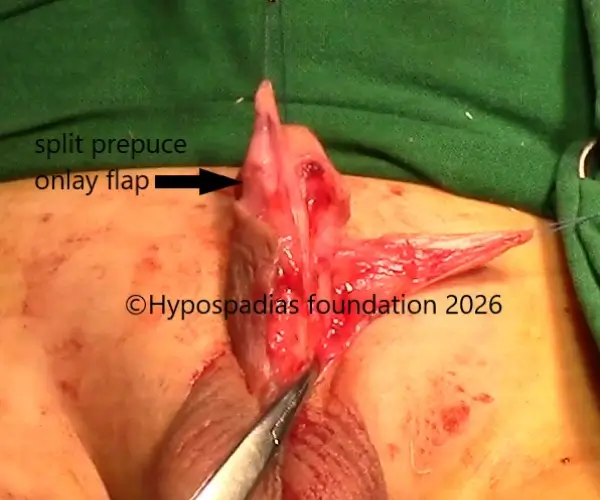
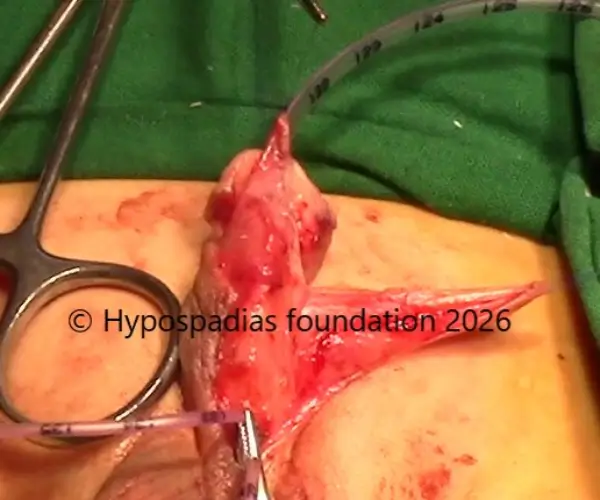
Pic 5: Split prepucial flap sutured to the edge of the urethral plate. Dartos flap spread fixed on either side of suture line
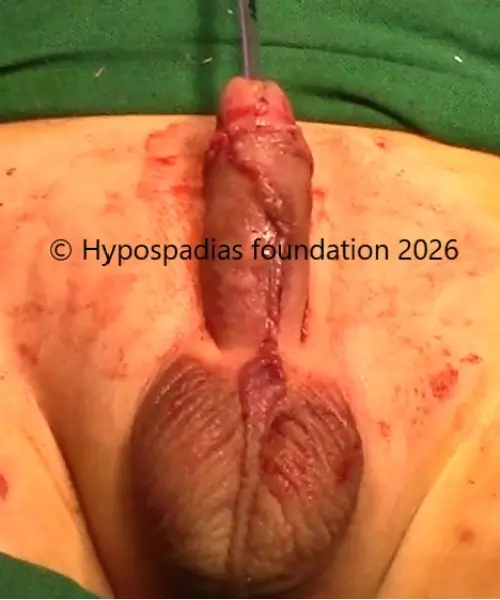
Pic 6: Modified split prepucial onlay flap repair complete

Pic 7: Cosmetic result at 1 month after surgery

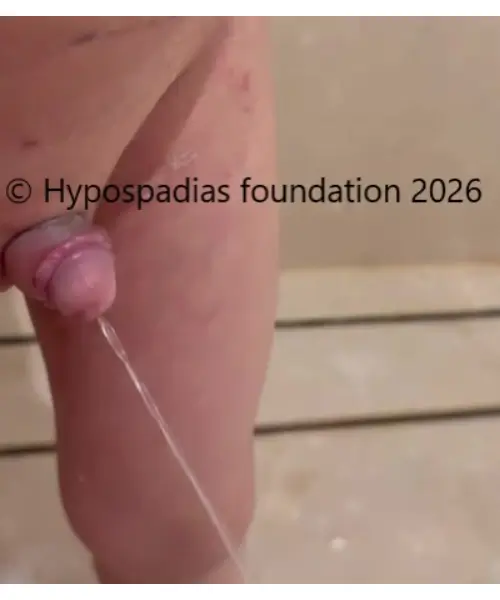
Pic 8: Appearance at 6 months after surgery with good urine stream
Single-Stage Repair of Proximal Penile Hypospadias with Split Preputial Onlay Flap Urethroplasty
Proximal Penile Hypospadias is a congenital condition in which the urethral opening (meatus) is in the proximal penile region rather than at the tip of the glans. Surgical management involves correction of penile curvature (chordee correction) and reconstruction of the urethra to bring the urinary opening to the tip of the penis. Early surgical correction is important to preserve normal urinary function and future sexual function.
Most pediatric urologists and hypospadias surgeons prefer a two-stage repair for proximal penile hypospadias, particularly in cases where:
1. Chordee is significant
2. The urethral plate is narrow or of poor quality
3. A long segment urethral reconstruction is required
However, a single-stage repair may be considered when the chordee after penile degloving is mild. In the present case, intraoperative assessment showed chordee of less than 30°, which allowed us to proceed with a single-stage reconstruction.
For urethral reconstruction, we used a modified preputial onlay flap urethroplasty (split preputial onlay flap). This technique is particularly useful in cases where chordee is mild, but the urethral plate is narrow or suboptimal. In this method, a well-vascularized flap from the dorsal prepuce is mobilized and sutured onto the urethral plate to form the neourethra. Preservation of the urethral plate combined with the addition of vascularized tissue helps create a wide and well-supported urethral channel.
This type of repair is technically demanding and generally yields good outcomes only when performed by experienced surgeons. The main advantage of this technique is the creation of a wider urethral lumen, which may reduce the risk of Urethral Stricture in the future.
However, potential complications may still occur, including:
Meatal Stenosis
Urethral Diverticulum
Urethrocutaneous Fistula
Careful patient selection, meticulous surgical technique, and adequate postoperative care are essential to achieve optimal outcomes in single-stage proximal hypospadias repair.
About Hypospadias Foundation
The Hypospadias Foundation, located in Kharghar, Navi Mumbai, Maharashtra, India, is recognized as one of the best hospitals centers for Hypospadias Surgery treatment in India and worldwide. Patients travel to the Hypospadias Foundation not only from across India but also from Asia, the Middle East, Africa, Europe, and North America seeking expert care for primary hypospadias repair, failed hypospadias surgery, and complex redo hypospadias cases.
Over the past 18 years, the Hypospadias Foundation has performed more than 5000 hypospadias surgeries every year, making it one of the highest-volume hypospadias centres in India and the world. With a complication rate of less than 5%, the centre has achieved
excellent surgical outcomes and international recognition in hypospadias management.
Expert Hypospadias Surgeons in India
Dr A. K. Singal is well experienced and respected hypospadias surgeon, and is rated as the best hypospadias surgeon in India and the world. He has dedicated his career to treating children and adults with hypospadias, including complex and failed repairs. His expertise in advanced hypospadias surgical techniques and reconstructive pediatric urology has helped thousands of patients achieve successful outcomes.
Dr Ashwitha Shenoy is an expert pediatric surgeon with a special interest in pediatric urology and hypospadias surgery. She works closely with Dr. Singal in managing both primary hypospadias cases and complex redo surgeries.
Together, Dr. Singal and Dr. Shenoy provide world-class hypospadias treatment in India, combining advanced surgical techniques, high surgical volume, and meticulous postoperative care. Their collaborative approach has resulted in excellent outcomes for children and adults undergoing hypospadias repair. Today, the Hypospadias Foundation in Navi Mumbai is widely regarded as a global referral centre for hypospadias surgery, helping patients achieve normal urinary function, improved cosmetic outcomes, and better quality of life.

