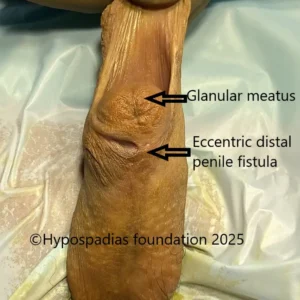
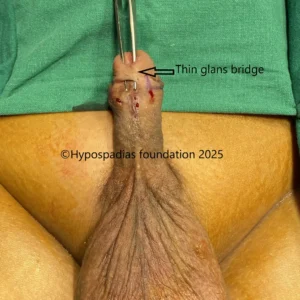
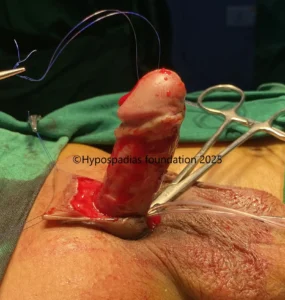
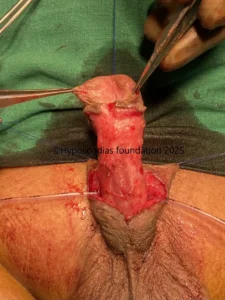
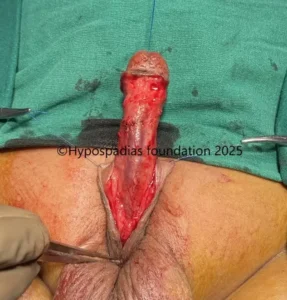
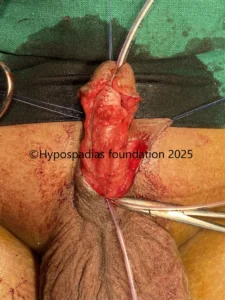
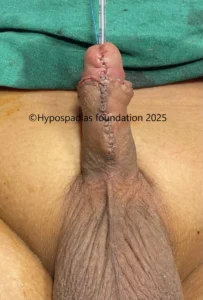
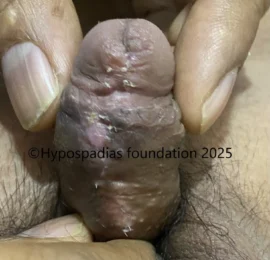
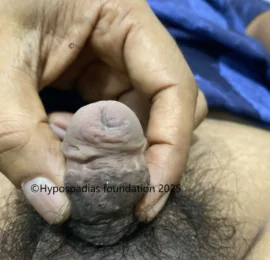
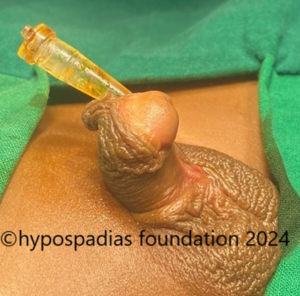
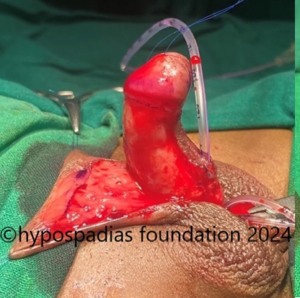
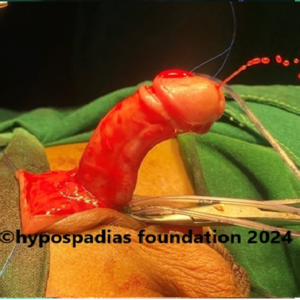
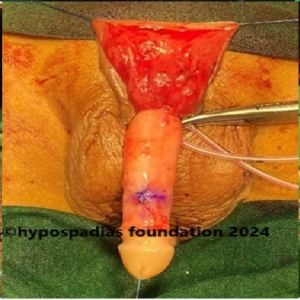
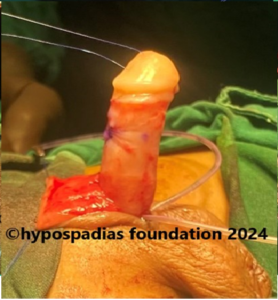
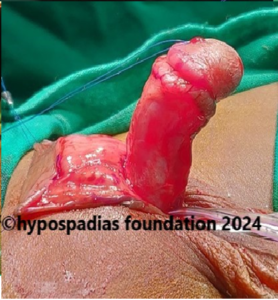
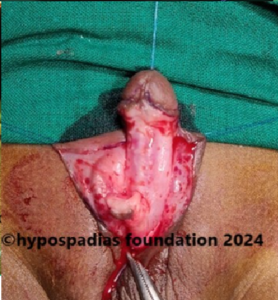
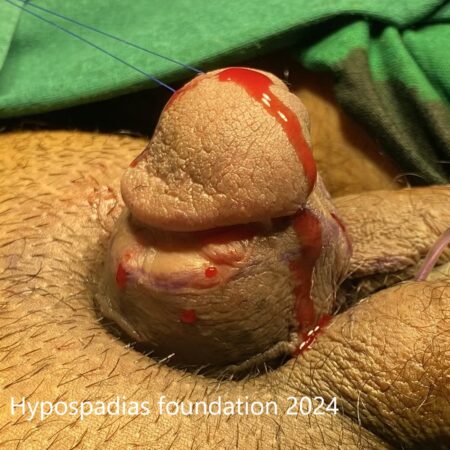
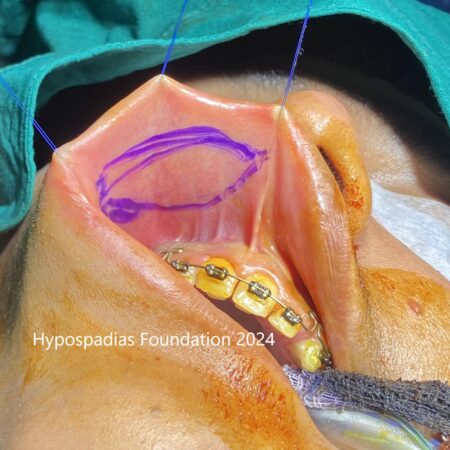
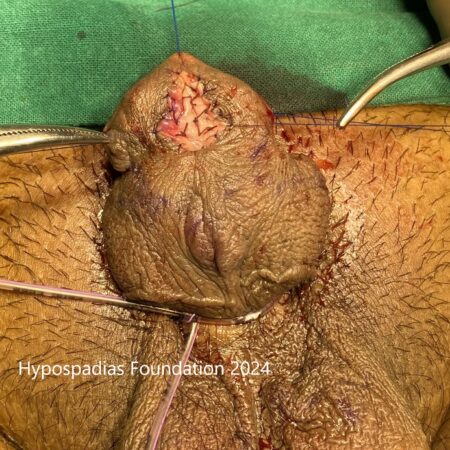
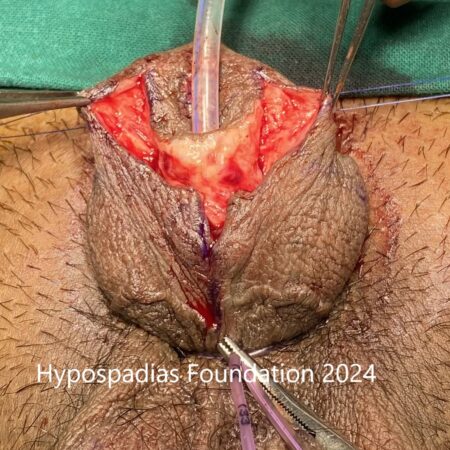
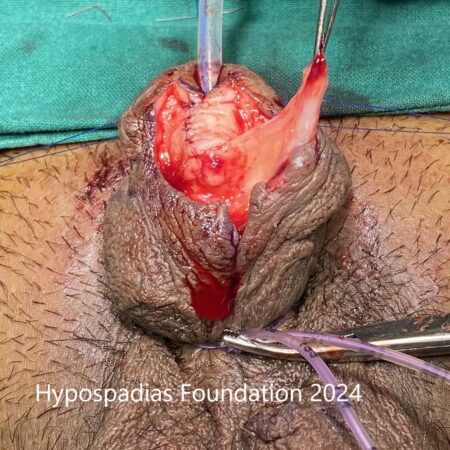
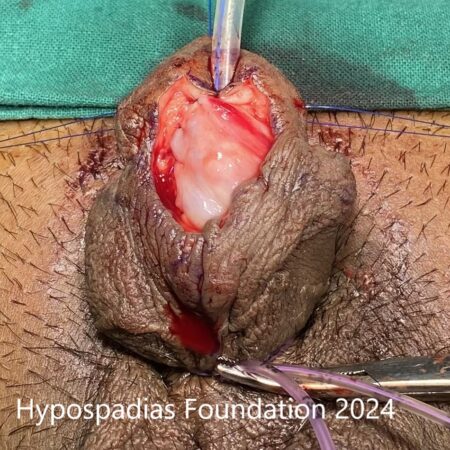
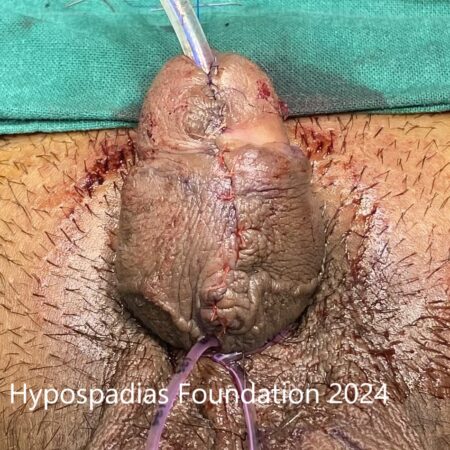
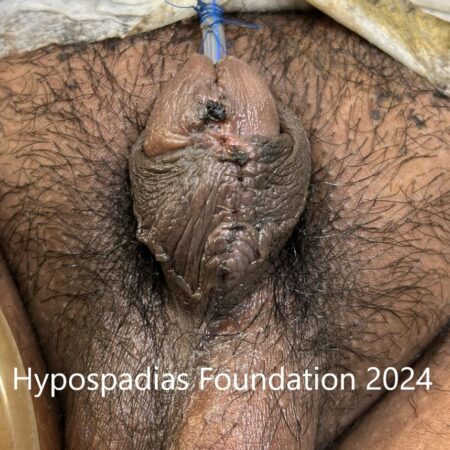
Hypospadias is a common congenital condition in boys where the urinary opening (urethral opening) is located on the underside of the penis instead of the tip. Hypospadias surgery is usually performed in early childhood, ideally before the age of five.
After successful hypospadias repair, the penis appears similar to a circumcised penis with urinary opening on tip and no curvature. The child will be able to pass urine in a single straight stream from the tip of the penis without pain or difficulty.
Because the surgery is performed very early in life, many children do not remember the condition or the procedure. As a result, many parents wonder:
Should we tell our child about his hypospadias surgery?
The answer is yes—open communication is important for your child’s long-term emotional and medical well-being.

Why parents have difficulty in talking to their son about hypospadias?
Many parents struggle with discussing hypospadias with their child due to social and emotional concerns such as
1. Cultural Taboo Around Genital Health
In many families, conversations about genitals or sexual health are considered uncomfortable or inappropriate. Parents who grew up in such environments may find it difficult to discuss these topics openly.
2. Fear of disclosure leading to social judgement and stigma
Parents often hesitate to disclose such conditions to their child due to fear that the child might share it with others, leading to social judgment. They may worry about teasing, stigma, or misunderstandings from peers, relatives, or the wider community. Concerns about how
the information could affect the child’s social relationships, self-esteem, and even future aspects like marriage or fertility can make parents cautious. As a result, some choose to delay or limit discussions, hoping to protect the child from potential negative reactions.
3. Concern About the Child’s Emotional Reaction
Some parents fear that their child may feel embarrassed, feel different from others, or become emotionally distressed if he learns about his hypospadias condition. Although these concerns are understandable, keeping the condition completely hidden may lead to problems later in life.
Why It Is Important to Tell Your Child About Hypospadias
1. Prevents Trust Issues
Children may eventually discover their medical history through records, online searches, or medical consultations. Learning about hypospadias surgery later in life from another source may make them feel betrayed or confused. Hence open communication is necessary to build trust and prevent unnecessary anxiety.
2. Reduces Body Image Concerns
As boys grow into adolescence, they naturally become more aware of their bodies. If they notice that their penis looks slightly different without understanding the reason, it may lead to unnecessary insecurity.
3. Prevents Anxiety During Puberty
Puberty brings many physical and emotional changes. Understanding their medical history helps adolescents feel confident and reduces anxiety about their bodies.
4. Helps With Healthy Relationships in Adulthood
Men who are unaware of their hypospadias repair history may feel worried or embarrassed about their appearance during intimate relationships. Knowing the truth early helps build confidence and reduces fear of judgment.
5. Seek help if they have medical issues
While with current hypospadias surgery techniques, the long-term results are very good, some of the children may develop issues in adulthood related to hypospadias or surgery done in childhood. These issues may include stricture, diverticulum, recurrent chordee or rarely urinary infections. Hence, it is important that the parents handover the medical records and tell their child about surgery so that they can seek proper help should anything happen.
6. Future urological interventions
Even in men without prior hypospadias, some of them develop kidney stones or prostate issues in late adulthood. At time of intervention, there is often cystoscopy done via urethra. Hence, it is important for them to know that they have a reconstructed urethra and share the same surgery record with their treating adult urologist.
What Is the Right Age to Talk About Hypospadias?
The best time to discuss about hypospadias with your child is during adolescence. At this stage, teenagers are mature enough to understand medical information and can process the explain logically.
Parents can explain that:
He was born with a small difference in the position of the urinary opening.
A hypospadias surgery was performed in childhood to correct it.
The condition has been successfully treated. It will not affect his normal life, urination, or future relationships. Having this conversation in a calm and supportive manner helps the child feel reassured and informed.
Why Medical Records of Hypospadias Surgery Are Important
When your child becomes an adult, it is important to provide him with all documents related to his hypospadias repair surgery. These records can help doctors if he ever needs medical evaluation later in life. Although most boys who undergo hypospadias surgery in childhood live completely normal lives, some rare complications can occur in adulthood, including:
1. Urethral Stricture: The reconstructed urethra may become narrow over time, affecting urine flow.
2. Urethral Diverticulum: The reconstructed urethra may become slightly dilated or relaxed.
3. Residual Chordee: A mild curvature of the penis that was not fully corrected in childhood may become more noticeable in adulthood.
Having the surgical history and medical records helps doctors provide appropriate treatment if any issue arises.
Who Should Explain about Hypospadias to the Child?
The best approach is for parents to have the conversation along with the hypospadias surgeon.
Together, they can reassure the child that:
The condition was corrected successfully.
He can lead a completely normal life.
If he has questions or concerns, he can discuss them privately with the doctor.
We also recommend a follow-up consultation around 18 years of age so that the young adult fully understands his medical history and can address any concerns.
Final Thoughts
Talking to your child about hypospadias and hypospadias surgery may feel uncomfortable at first, but open and honest communication is important. When parents discuss the condition At the right age, it helps build trust, confidence, and a healthy body image. Providing accurate information ensures that your child grows into adulthood feeling reassured, informed, and comfortable with his medical history.
About hypospadias foundation
Hypospadias Foundation, located at MITR Hospital in Kharghar, Navi Mumbai in the state of Maharashtra, India is a centre specialized for the treatment of children and adults with hypospadias. Our expertise in hypospadias makes us one of the best centres for hypospadias repair in the world. We treat children from more than 30 countries in the world and from all over India. Our dedication in this field has helped us achieve excellent outcomes.
Dr A K Singal is an expert and top hypospadias surgeon in India. He is a gifted surgeon and his expertise in this area has helped us achieve excellent outcomes in primary and failed hypospadias in children as well as adults. Dr Ashwitha Shenoy is an expert hypospadias surgeon with a special interest in hypospadias and pediatric urology. Both Dr Singal and Dr Shenoy work together to give best results for hypospadias surgery in India for both children and adults.
Contact Form for Hypospadias Foundation
Please fill all clinical details and upload pictures and clinical summaries (if available)